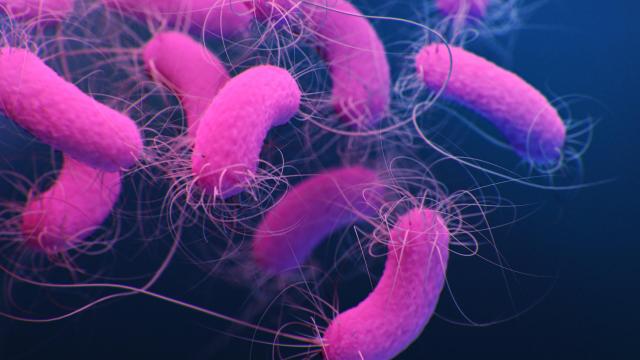
One person’s extra snot is a bacteria’s treasure, a team of scientists say. In new research, they detail how a common opportunistic germ can manipulate our immune system into producing mucus when it shouldn’t. The clever trick not only allows the microbe to avoid destruction but also gives it a rich source of fuel to keep growing.
The bacteria is Pseudomonas aeruginosa. It’s commonly found in the environment, particularly the soil, but it also frequently makes a home in living organisms, humans included. Normally, these rod-shaped bacteria don’t cause health problems when colonising the human body. In people with weakened immune systems, however, they can grow out of control and cause chronic, even life-threatening infections. If that’s not bad enough, P. aeruginosa is naturally hardy against many antibiotics, and some strains have learned how to resist them even more over time. Multidrug-resistant infections of P. aeruginosa are a major concern in hospitals and are thought to kill at least 2,700 Americans a year.
Germs have evolved all sorts of methods to evade and survive the defences of their hosts. There are, broadly speaking, two different ways that our immune system responds to a germ: one that it reserves for acute infections like those caused by bacteria and viruses (type 1 immunity) and another that it usually uses against lingering parasites like tapeworms (type 2 immunity). Some germs have learned how to convince the immune system to use the wrong type of response, a strategy called immune deviation. The authors of this current study, published Wednesday in the journal Immunity, theorised that P. aeruginosa is one such germ and wanted to find out how it pulls off this deception.
To do so, they studied how the bacteria interacted with mouse and human airway cells in the lab. The germ can release a toxin called LasB. And in these cells, the team found, LasB can set off a chain reaction that triggers a type 2 immune response, characterised by inflammation and the production of mucins, the key components of mucus. When they neutered the bacteria to not produce LasB, this immune response was muted. Other experiments showed that the bacteria likes to eat human mucus. Put all together, the team’s work suggests that P. aeruginosa can turn us into a snot factory, mainly with the help of LasB, using that very snot to keep itself alive and thriving.
“Our study thus reveals a type of bacterial immune deviation by increasing nutrient supply,” the study authors wrote.
The findings don’t just showcase a gross example of how germs can take advantage of us for survival. Type 2 immunity also plays a role in causing allergies, which happen when the body overreacts to a foreign substance that’s actually harmless. And the team’s experiments with mice found that P. aeruginosa and LasB can actually amplify the typical allergic reaction. That finding could have some important implications for people chronically infected with P. aeruginosa, such as patients with cystic fibrosis.
In the long term, the authors say, this kind of work might help us better understand how chronic infections like those caused by P. aeruginosa interact with our immune system and other aspects of our body, including the gut microbiome. And perhaps someday, it could bring scientists closer to developing better drugs for them — an urgent priority in an era when we’re increasingly running out of reliable antibiotics.