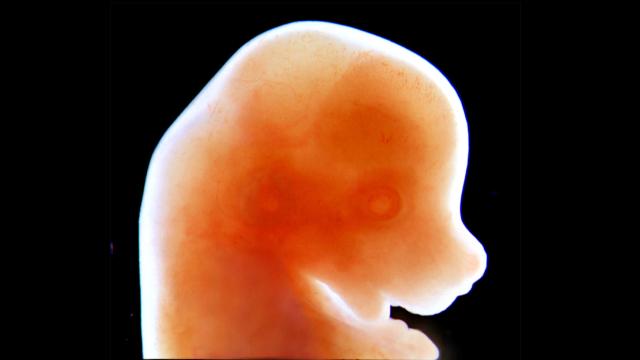
Quivering with life, the developing mice moved ever-so-slightly in their vials. Just a few days since they were fertilised, the rodent embryos were minuscule — smaller than an Aspirin tablet — but their existence a is monumental feat: they developed in an artificial uterus, a first in early mammalian science and a big step in improving scientists’ understanding of embryonic development.
The research, published today in the journal Nature, describes how the scientists took new embryos and developed them over the course of six days, about a third of the total mouse gestation period, outside of a rodent uterus.
“If you give an embryo the right conditions, its genetic code will function like a pre-set line of dominos, arranged to fall one after the other,” said co-author Jacob Hanna, a developmental biologist at the Weizmann Institute of Science in Israel, in a Weizmann Institute of Science release. “Our aim was to recreate those conditions, and now we can watch, in real time, as each domino hits the next one in line.”
For nearly a century, scientists have tooled around with the idea of taking mammalian embryonic development outside the uterus, in order to better understand how our cells come together and swiftly shape themselves into organisms. For much of that time, though, delving into the earliest stages of that development has been a black box; later stages can more easily be simulated, as they were in 2017, when a group used a bag-like device to incubate lambs to delivery in Philadelphia.
Two years later, that same team announced they could keep preterm fetal lambs alive in an artificial womb. Following their delivery, the premature mammals looked just as healthy as their on-time counterparts. “In the world of artificial placenta technology,” said one of the study authors at the time, “we have effectively broken the 4-minute mile.”
Those lambs were vastly more developed than the newly observed mice. The germinal stages of all mammalian life are difficult to observe in-utero, so biologists and geneticists previously pieced together an idea of what goes on by combining observations, such as looking at amphibian’s external eggs and comparing them with images of dissected mouse embryos. The recent work changes that.
[referenced id=”1059876″ url=”https://gizmodo.com.au/2017/08/australian-researchers-have-used-an-artificial-womb-to-incubate-a-lamb-for-the-second-time/” thumb=”https://gizmodo.com.au/wp-content/uploads/2017/08/19/nx3ydsqs8v8jk12htluf-300×169.png” title=”Australian Researchers Have Used An Artificial Womb To Incubate A Lamb For The Second Time” excerpt=”It may look like a glorified Ziplock bag, but the artificial womb could one day save the lives of the thousands of babies born prematurely every year.”]
The initial mouse embryos consisted of just a few hundred cells and were placed on laboratory dishes mimicking the uterine wall. After a couple of days, the team moved the embryos into beakers filled with a nutrient solution and regulated the oxygen and carbon dioxide amounts and pressure of the embryos’ new environment. After about six days, the embryo’s growth was unsustainable, and they were destroyed before they came to term.
There are a couple of hurdles Hanna hopes will be taken on next: The embryos needed a blood supply, and they still had to be fertilised and initially grown in a rodent uterus. In future experiments, Hanna hopes to somehow incorporate artificial blood and to synthesise embryos from stem cells to avoid the need for a biological uterus altogether.
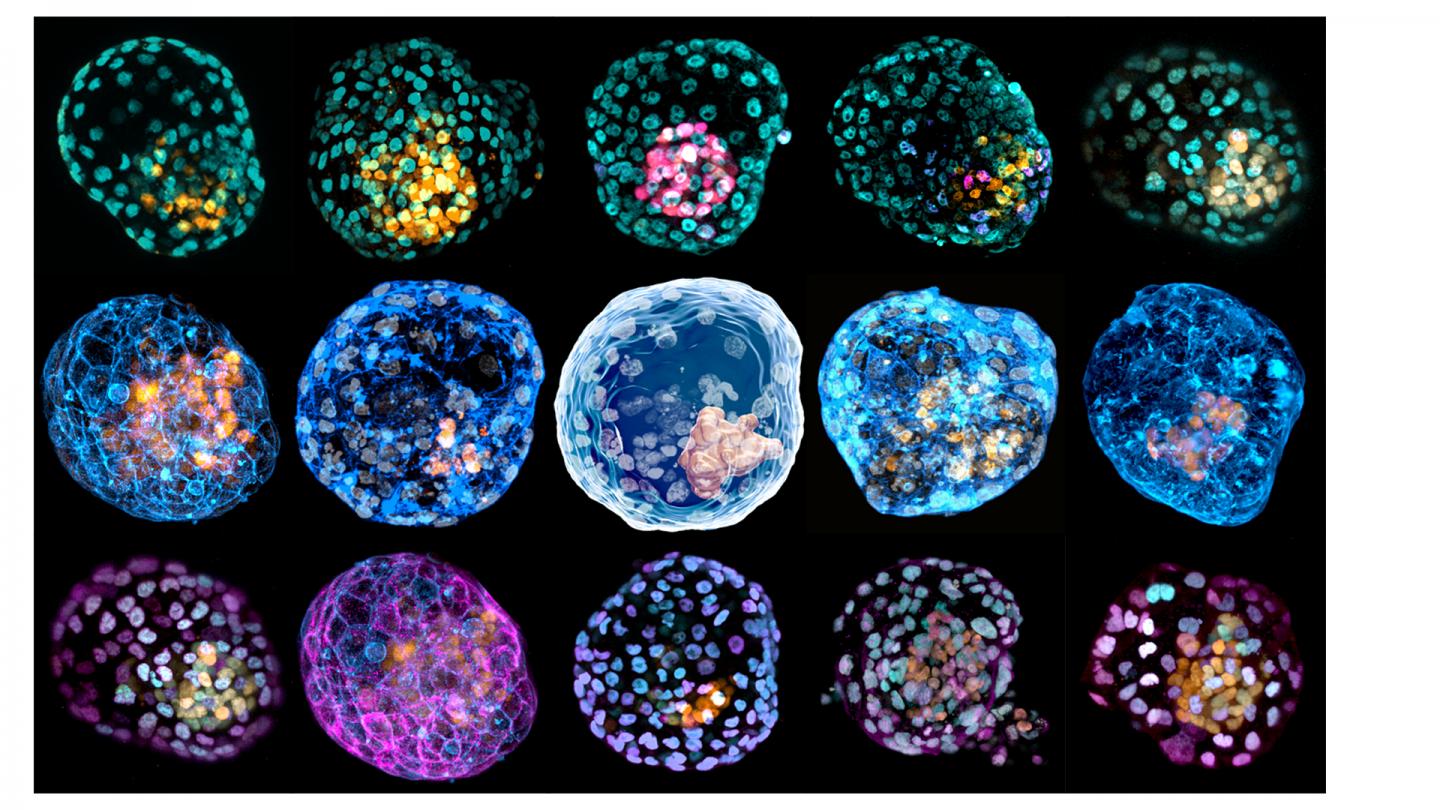
The new research was published in conjunction with another paper in Nature today; that work describes an early human embryo model generated from skin cells. The research team was able to reprogram human skin cells into structures similar to blastocysts, the embryonic stage that occurs about five days after an egg’s fertilisation. The synthetic structures, called iBlastoids (as if through some bizarro collaboration between Apple and Pokémon), have significant implications for understanding infertility, the conditions that cause miscarriages, and other aspects of early human development.
“iBlastoids will allow scientists to study the very early steps in human development and some of the causes of infertility, congenital diseases and the impact of toxins and viruses on early embryos,” said co-author Jose Polo, a developmental biologist at Monash University in Australia in a university press release, “without the use of human blastocysts and, importantly, at an unprecedented scale, accelerating our understanding and the development of new therapies.”
Just as watching replays of races will inform a runner on how to improve their technique, being able to replicate and observe the primary stages of mammalian life many times over will help scientists understand how to improve conditions for life at its beginning.