Researchers say they may have found a way to create more useful fat cells using the gene-editing technique CRISPR. In a new study out Wednesday, they found evidence — in mice — that these engineered cells can possibly help the body burn calories quicker, as well as prevent obesity and other metabolic problems, compared to the fat cells most commonly found in the human body. But the findings are still a long way from being applicable to people.
Yu-Hua Tseng, a diabetes researcher at Harvard Medical School, and her lab have been studying the intricacies of fat cells for years, focusing on the difference between so-called white and brown fat cells (the brown colour comes from the higher amounts of mitochondria they have, which contain lots of iron). The primary purpose of white fat cells is to store energy from food, while brown fat cells are thought primarily to be used as a way to keep our body temperature stable, particularly in the cold.
Scientists like Tseng have shown that brown fat cells are better at breaking down the nutrients they process than white fat. But most fat in the body is white, not brown, and many people now have an overabundance of body fat, leading to health problems like obesity and type 2 diabetes. As a result, Tseng and her team have theorised that if we find a way to safely make white fat cells more brown-like, that should help treat or prevent obesity.
In this new study, published Wednesday in Science Translational Medicine, Tseng and her team appeared to do just that. With the help of CRISPR, they made changes to precursor human white fat cells. The changes enabled the white fat cells to express a protein usually produced by brown fat cells and thought to be key to their improved energy-burning ability, known as uncoupling protein 1 (UCP1). Then they transplanted these human brown-like cells — codenamed HUMBLE cells — into obese mice fed a high-fat diet and documented to what happened to them compared to a control group of mice that were given human white fat cells via transplant and a third group of mice with transplanted brown fat cells.
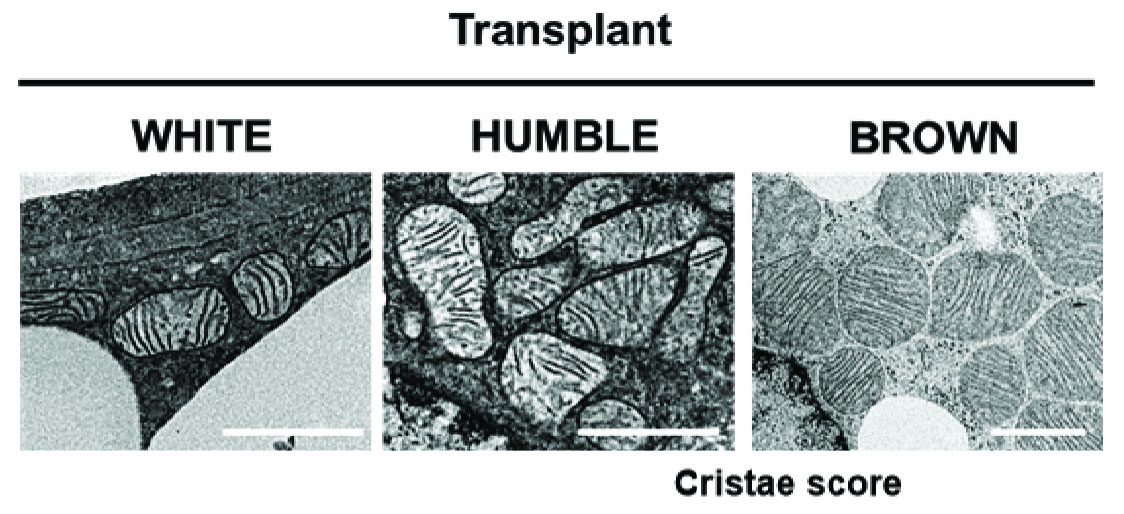
Tseng and her team found that the mice with HUMBLE cells were better off across the board than the mice with white fat cells and had similar outcomes to the mice with brown fat cells. The internal structure of HUMBLE cells also more resembled brown fat cells, particularly when it came to their mitochondria.
“They’re able to clear their glucose much quicker; they’re able to better respond to insulin. And in terms of weight gain, they can gain less weight compared to the control mice,” Tseng said by phone. “So all that signifies an improvement to their metabolism.”
These experiments are a proof-of-concept for researchers like Tseng, not something that will be tested in humans in clinical trials anytime soon. We’re only now starting to see the very first, small trials of CRISPR in people for diseases like cancer and muscular dystrophy, though results have been so far encouraging.
There are inherent limitations to the approach Tseng and her team used in this study. For instance, the mice were immunocompromised to ensure that the human cells would be accepted without any problems. The cells used were also cultivated from the cell lines of only two people. It’s possible that a native immune system might affect how HUMBLE cells work, as could harvesting these cells from a larger number of people, the authors noted.
But by successfully creating these cells and studying how they made the mice healthier, Tseng said, we’ll get that much closer to finding an effective way to help people reduce or prevent obesity. This could happen through genetic engineering or via a drug that can mimic its effects on white fat cells, she added. Already in this study, the team found evidence that these HUMBLE cells ramp up the production of nitric oxide in the blood, which in turn may activate native brown fat cells elsewhere in the body (in other research, lowered nitric oxide production has been linked to obesity).
Aside from studying these HUMBLE cells more closely in the lab, Tseng is also looking to collaborate with researchers and clinicians in other fields.
“To be able to apply this to patients someday, we need a team with diverse expertise. I certainly cannot accomplish that myself,” she said. “But I really do hope that our research can benefit patients eventually.”
