New research published this week may help radiologists identify survivors of domestic abuse through the study of X-rays.
Researchers from the Departments of Radiology and Emergency Medicine at the Brigham and Women’s Hospital, as well as a researcher from the Department of Biostatistics at Harvard’s T.H. Chan School of Public Health, conducted a pilot study to determine whether X-rays could be used as a possible indication of domestic violence.
They looked at the electronic medical records of 185 patients referred by the emergency department to the intimate partner violence (IPV) support program between January 2015 and October 2016. These patients were compared with an age and sex-matched control group of 555 patients from the emergency department.
The study found a number of distinctions between the two groups. For instance, survivors of intimate partner violence were found to have received about four times as many imaging studies as patients from the control group.
According to the research, half of the extremity fractures observed in the IPV patients occurred in the upper extremity, while the majority of fractures occurring in the control group affected the lower half of the body.
“This could reflect a mechanism of accidental trauma in the control group, while craniofacial fractures allude to a nonaccidental mechanism of trauma,” the researchers wrote.
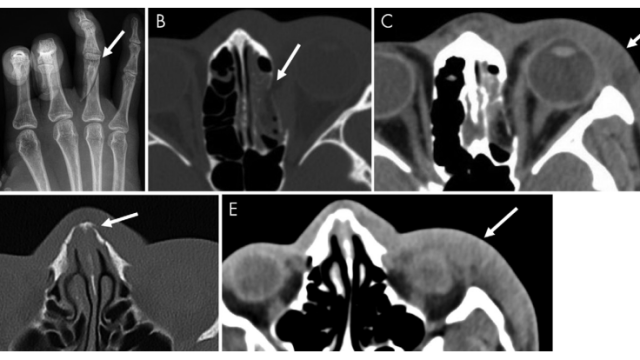
The study also notes that nine out of 11 of the head and neck fractures in patients who experienced intimate partner violence happened in the nasal bone or orbit.
Amber Mitchell, a phone services advocate for the US National Domestic Violence Hotline and loveisrespect, told Gizmodo that this study “provides some interesting context about how domestic violence can look in a hospital setting,” adding that “this correlation could help medical professionals help identify some red flags or warning signs that they may be dealing with someone who is a victim of intimate partner violence”.
Patients of intimate partner violence were also more likely than the control group to experience obstetric complications, chronic fractures of the extremities and nasal bone, and subacute fractures. The researchers wrote in the paper that the latter two “could be reflective of ongoing repetitive trauma”.
According to the study, 81.6 per cent of the survivors of intimate partner violence reported a previous history of violence.
The findings in the study also indicate that 96 per cent of the survivors of intimate partner violence were women. They also had a higher likelihood of experiencing homelessness or a psychiatric illness.
While the study found that intimate partner violence affected all racial backgrounds, there was a higher proportion of African American and Latinx patients.
Bharti Khurana, the director of Emergency Musculoskeletal Radiology at Brigham and Women’s Hospital and an author of the study, told Popular Science that she wants to build a tool for radiologists that would inform them if a patient’s X-ray and electronic medical record history pointed to intimate partner violence. This would allow the radiologist to inform the patient’s physician or bring in a social worker.
“One thing that we hear really commonly at the hotline is being unable to speak with a medical professional because their partner might be present, so there’s always some concerns around safety, can they even tell a doctor what’s going on?” Mitchell said.
She said that if a doctor suspects abuse, “if there are inconsistencies about the stories that don’t match up with the injury”, that they can figure out a way to get the patient alone and to use that privacy to ask if they are safe and if they need help.
“Another one we hear really frequently is fear of even seeking medical attention,” Mitchell said, as they may be worried about steps a hospital will take without the patient’s consent.
She said that if a medical professional does suspect their patient might be a victim of domestic violence, they can inform them of their confidentiality and the steps they can take, allowing the patient “to make an informed decision”.
“I think it’s great to have people looking into this and knowing that the hospitals can be a resource for people who are experiencing violence,” Mitchell said, “bringing in social workers or developing a safety plan, that can be really helpful.”
If domestic violence is affecting you or someone you know, call 1800 RESPECT or visit White Ribbon Australia‘s website.