Incubators and ventilators are invaluable when treating extremely premature infants, but they’re a far cry from the cosy confines of a mother’s womb. In an effort to create an environment that more closely approximates the real thing, researchers have now developed an artificial womb that could dramatically reduce mortality and disease in preemies.
Image: Karen Abeyaseker / Creative Commons
The research team, led by Alan Flake from the Children’s Hospital of Philadelphia, has shown that it’s possible to support extremely premature lambs in an external artificial womb, and to recreate the conditions required for normal gestational development. The lambs were able to grow inside a fluid-filled device, which sustained them for a record-breaking four weeks. Subsequent tests on the lambs indicated normal development of their brain, lungs and organs. It may take another decade before this technology can be used on premature human infants, but it’s an important step in that direction. The details of the new study can be found in Nature Communications.
Each year in the United States, approximately 30,000 births are critically preterm, meaning babies are born before 26 weeks of gestation (normal gestation is 37 weeks). In Australia, around 0.8 per cent of babies are born after only 20 to 27 weeks of gestation. Extreme prematurity is the leading cause of infant mortality and disease, causing a third of all infant deaths and half of all cerebral palsy diagnoses attributed to preterm births. But medical practices are steadily improving, pushing the limits of viability outside of the womb to 22 to 23 weeks of gestation. These tiny babies, who often weigh no more than 600g, have about a 30 to 50 per cent chance of survival. Around 90 per cent of those who do survive experience health-related complications, such as chronic lung disease and complications arising from poor organ development.
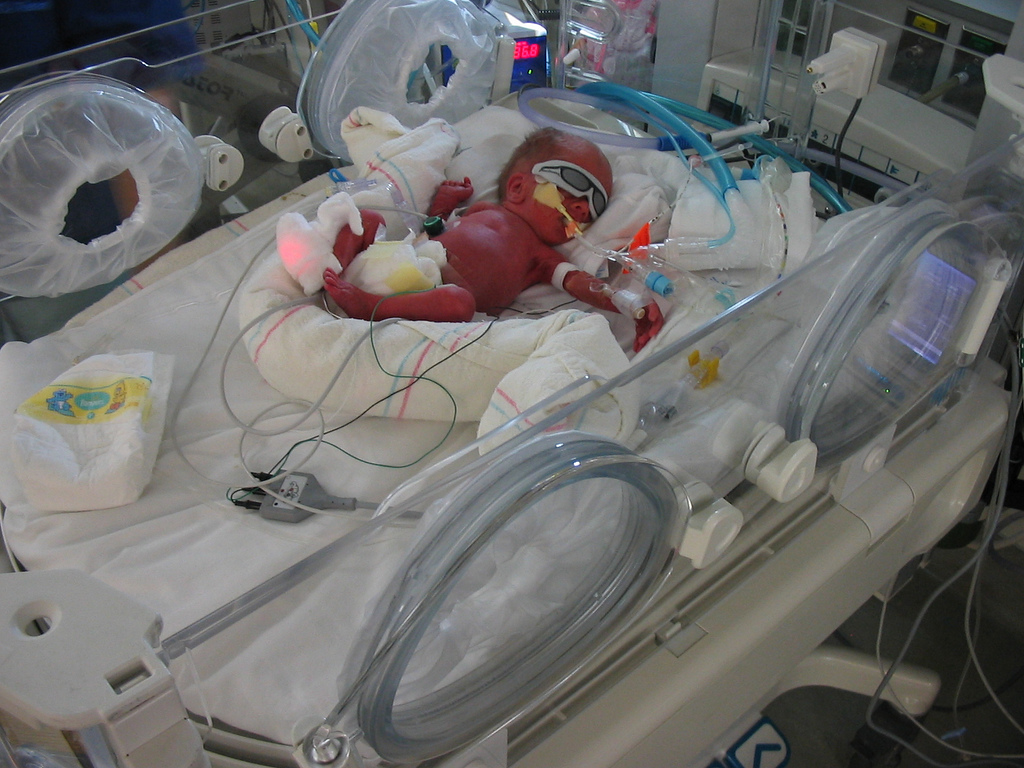
The conventional approach to treating preemies. (Image: The Hudson Family/Flickr)
Currently, the best we can do for these premature infants is place them in an incubator and assist their still-developing bodily functions. “Conventional care involves supporting organ functions, intubation, mechanical respirations, and gas based ventilation of lungs,” noted study co-author Emily Partridge at a press conference held yesterday. “Normally, lungs are submerged in fluid [in the womb], but gas-based methods impair lung development, causing lifelong health issues.” In addition to being tough on the preemie’s lungs and developing organs, these standard treatments can expose infants to infectious pathogens.
The new system is an effort to move away from this clumsy approach and simulate the conditions in the mother’s womb as closely as possible. In experiments, Flake and his colleagues used a semi-closed, fluid-filled artificial environment consisting of a polyethylene “Biobag” that uses the infant’s umbilical cord to create an oxygen circuit.
Following a C-section, six premature fetal lambs were placed in their own plastic containers (lambs were used because prenatal lung development in lambs is very similar to that of humans). The lambs grew in the device as they normally would, developing in a temperature-controlled, near-sterile environment. They breathed in amniotic fluid, while their hearts pumped blood through their umbilical cords into a gas exchange system outside of the bag. Electronic monitors measured their vital signs, blood flow and other important functions.
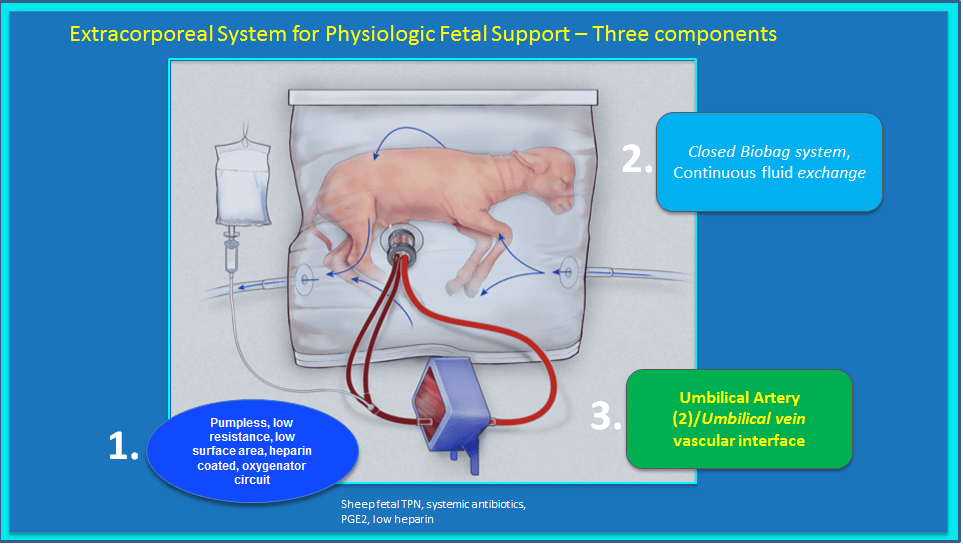
Image: Children’s Hospital of Philadelphia.
The lambs, which were at the biological equivalent of the 23 to 24 week gestation stage of premature human infants when the experiment started, developed normally, marking the first time scientists have ever achieved this outside of the womb. “We’ve been amazed at how well this has worked,” commented Flake at yesterday’s press conference.
Unlike previous efforts, the new system doesn’t use an external pump to drive circulation; the fetus provides all of the power. This is important because even gentle artificial pressure can fatally overload an underdeveloped heart. As another bonus, the new system doesn’t require a ventilator. Instead, the baby’s heart pumps blood through the umbilical cord into the system’s low-resistance external oxygenator that substitutes for the mother’s placenta. The artificial amniotic fluid — an electrolyte solution manufactured in the lab — simulates the conditions inside the mother’s fluid-filled sac, allowing lungs and other organs to develop more naturally, while conferring protection from the outside world.
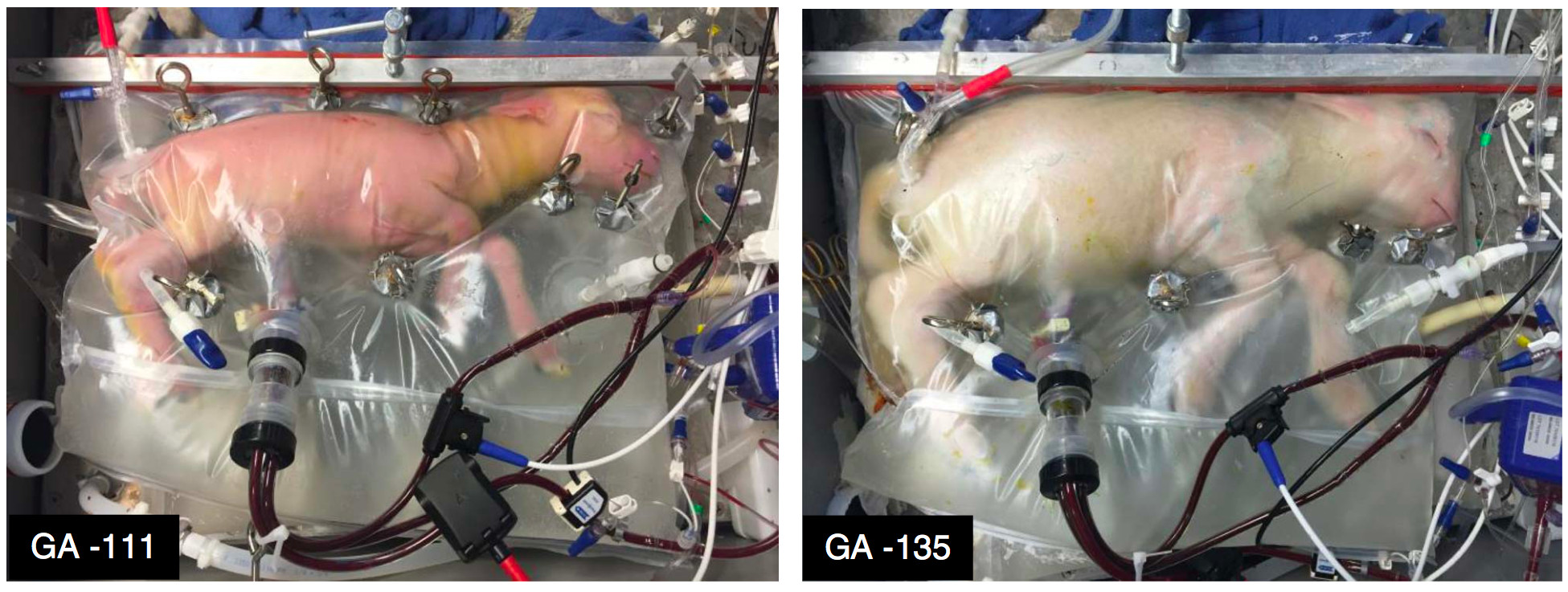
The Biobag system in use. The image on the left shows a lamb at 107 days of gestation and on day four of support. The image on the right shows the same lamb on day 28 of support. (Image: E.A. Partridge et al., 2017/Nature Communications
Prior to the new study, the maximum duration that a lamb fetus had been sustained in an artificial system was 60 hours, but the animals used in those experiments experienced brain damage. The new system has been demonstrated to work for at least 670 hours, or 28 days, pushing a 23 week-old preemie close to that critical 28 week stage. Follow-up tests on the lambs — including on some euthanised shortly after removal from the biobags — showed that they developed normally. As Flake put it, “In tests, the lamb’s… development caught up with normal fetuses.” The lambs exhibited normal blood pressure, circulation, metabolic parameters, growth, lung development and brain development. The oldest lamb is now a year old, and doing fine.
Importantly, the system is not meant to extend viability outside of the womb further back than 23 weeks. Nor is meant to bring a baby to full term. Rather, it’s a bridge between the mother’s womb and the outside world, supporting the infant from 23 weeks to 28 weeks of gestational age, after which time the effects of prematurity are minimal. Some scientists have speculated that eventually, we’ll able to sustain a fetus outside of the womb from the moment of conception straight through until a full term birth, but Flake stressed that their system has virtually nothing to do with this futuristic vision. “There is no technology, even on the horizon, that can support the fetus from the embryonic stage,” he said. “I would be very concerned if other parties wanted to use this device to extend viability [outside of the womb].”
The researchers said more work still needs to be done before their system can tested on human infants. For one, the system needs to be downsized. Lambs are reasonable approximations of humans, but human fetuses are about one third smaller than lambs. Flake said his team needs to make sure the self-driven pumps will work just as well for smaller bodies.
As a final note, the researchers stressed that their system won’t entail translucent bags of fetuses hanging from the walls of intensive care units. Once it’s ready for human use, the system would consist of a chamber filled with amniotic fluid. Like a normal womb, it would be closed off from the outside world. A special dark-vision camera would be placed inside, allowing medical staff and parents to monitor the baby over time. Other instruments would be used to monitor vital signs and other important health measures.
It may sound like a radical departure from the current incubator model — and it is — but the team has the right idea. The more we can approximate the conditions of the womb, the better, and a brand new approach to treating preemies is likely just the start.