For friends and family, fewer things are more agonising than not knowing if or when a loved one in a coma will regain consciousness following a severe head injury or drug overdose. Researchers have shown that a common test can measure awareness in comatose patients — and even predict when they might wake up.
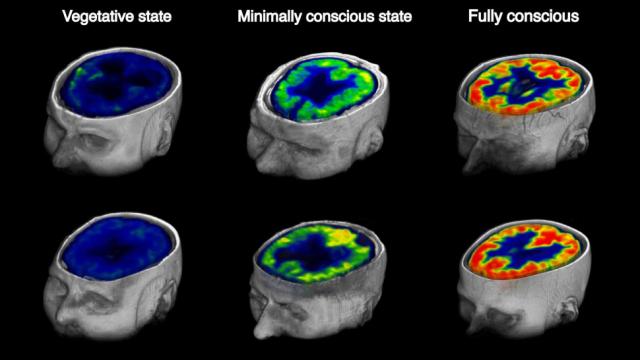
Glucose metabolism in the brain in patients with chronic disorders of unconsciousness. (Image: Stender et al., 2016)
As described in the latest edition of Current Biology, a readily available test that measures the amount of glucose (sugar) that’s being consumed by the brain can be used to help doctors tell the difference between patients in a full-on coma and those with partial or hidden signs of awareness. It can also predict whether or not they will recover awareness within a year.
For the most part, patients in a coma have lost their thinking abilities and are oblivious to their surroundings. But those in a so-called vegetative state often give the impression of someone who is emerging from a coma. Unlike a patient in a full coma, they’re in a state of partial arousal, but still lack full awareness. The new test — which is already available in virtually every hospital — will make it easier for doctors to assess the nature and severity of comas.
“In nearly all cases, whole-brain energy turnover directly predicted either the current level of awareness or its subsequent recovery,” said Ron Kupers of the University of Copenhagen and Yale University in a statement. “In short, our findings indicate that there is a minimal energetic requirement for sustained consciousness to arise after brain injury.”
To reach this conclusion, Kupers and his colleagues quantified and mapped cerebral sugar metabolism in 131 brain-injured patients, all of whom were suffering from either full or partial loss of consciousness. Using a well-known imaging technique known as FDG-PET, they were able to capture and map glucose uptake in the brain.
Results showed that a patient’s behavioural response was strongly linked to their overall cerebral energy turnover. Patients with a glucose metabolism below 42 per cent of normal activity appeared to be fully unconscious and did not recover consciousness after a year. But those who had brain metabolic activity above this critical threshold either displayed signs of partial awareness, or had awakened from their unconscious state a year later. Overall, the cerebral metabolic rate accounted for the imminent return of awareness in 94 per cent of patients.
“The discovery of a clear metabolic boundary between the conscious and unconscious states could imply that the brain undergoes a fundamental state change at a certain level of energy turnover, in a sense that consciousness ‘ignites’ as brain activity reaches a certain threshold,” said study co-author Johan Stender. “We were not able to test this hypothesis directly, but it provides a very interesting direction for future research.”
The scientists say that it will be important for other researchers to verify their findings in other sets of patients. Until then, they’re going to investigate how brain metabolism changes over time in brain-injured patients.