The history of inoculation may sound a little dry, but it’s really an epic tale of human trafficking, semi-illicit experimentation, and high explosives. It’s a globe-hopping story that stars harem girls, noblewomen, prisoners, princesses, slaves, and even a witch hunter.
In the Shadow of Smallpox
Smallpox has troubled humanity for thousands of years. Wherever we’ve settled in the world, the smallpox virus has eventually followed.
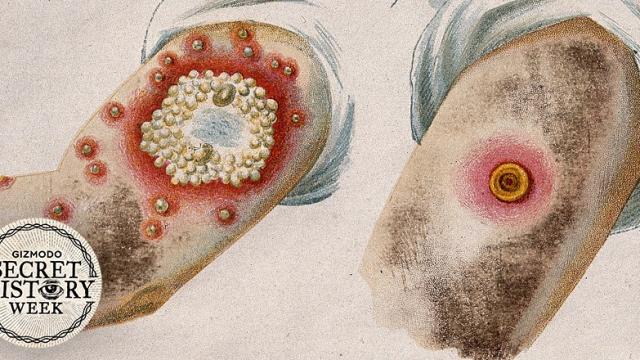
A dangerously high fever comes first, accompanied by headaches, back pain, and vomiting. Painful sores open in your mouth and nose, and a rash spreads all over your body. Blisters form and fill with pus; these pustules eventually scab over and dry up. About 30 per cent of people who catch smallpox will die; the rest will live with scars left behind by the pustules.
People eventually noticed one very important thing about smallpox: those who had survived didn’t catch the disease again, or if they did, they didn’t get very sick the second time around.
History doesn’t record who first got the idea to expose healthy people to pus from infected patients’ pustules – or how they talked anyone into letting them try it. But the practice seems to have sprung up independently in several places: India, China, West Africa, and elsewhere. The idea was already an old one in 570 AD when people in Europe started calling it “variolation,” from the Latin name for smallpox, Variola. (Later generations used “variolation” and “inoculation” interchangeably; today “inoculation” also includes vaccination.)
Variolation usually meant rubbing pus from a smallpox pustule – a good ripe one, the runnier, the better – into a cut or scratch on a healthy person’s arm, but in China, people just soaked a cotton ball in infected pus and stuck it up their noses. (Ah, the good old days, right?)
Most modern experts would consider this “stick it up your nose” strategy as the exact opposite of what you’re supposed to do with a deadly pathogen. But it was the best option available at the time, and it worked remarkably well. Only about two per cent of people who were exposed to smallpox through inoculation died of the disease, and only two to three per cent spread the infection to others. Today, that wouldn’t be an acceptable safety record for a vaccine, but in the 17th and 18th centuries, it beat the daylights out of a 15-30 per cent chance of dying if you caught smallpox on your own.
Herd Immunity and the Harem
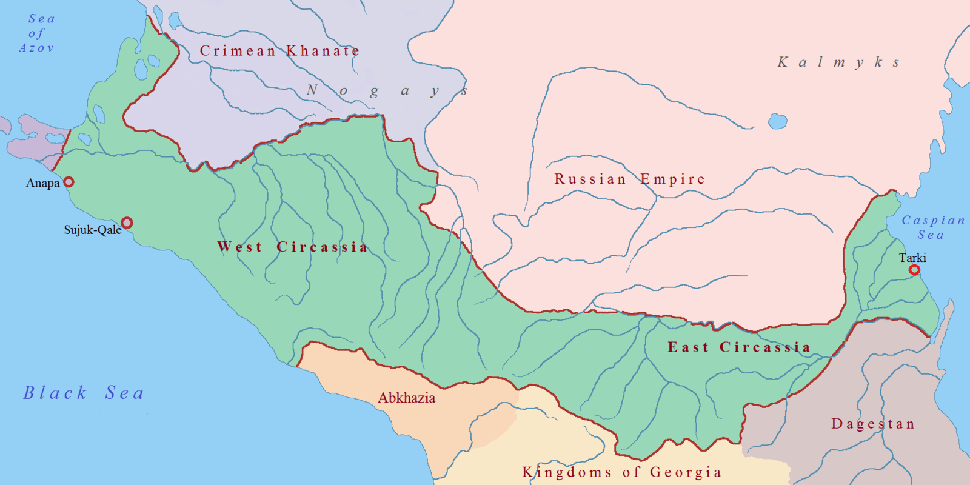
Circassia in 1700. Image: Adamsa123 via Wikimedia Commons
In the northern Caucasus Mountains, women of the Circassian ethnic group traditionally inoculated their children at about six months, and many Circassian women carried their knowledge with them when they were trafficked to Turkey as slaves – a common fate for many Circassians up until the early 20th century.
The French philosopher Voltaire described the situation in 1778:
“The Circassians are poor, and their daughters are beautiful, and indeed, it is in them they chiefly trade. They furnish with beauties the seraglios of the Turkish Sultan, of the Persian Sophy, and of all those who are wealthy enough to purchase and maintain such precious merchandise.”
The unfortunate Circassian women who ended up in the Ottoman Sultan’s harem left their mark on Turkish culture, one that would eventually spread across Europe and into North America. According to Voltaire,
“The Turks, who are people of good sense, soon adopted this custom, insomuch that at this time there is not a bassa in Constantinople but communicates the small-pox to his children of both sexes immediately upon their being weaned.”
According to some sources, inoculation first caught on in Turkey in the late 1600s, thanks to the Sultan’s trafficked Circassian women. Fifty years later, another woman carried the technique to England and eventually helped spread it throughout Europe.
A Woman on a Mission

Lady Mary Wortley Montagu in Turkish attire, painted 1756. Image: Wikimedia Commons
In December of 1715, Lady Mary Wortley Montagu was on top of the world, or at least her rather luxurious corner of it. She was the daughter of an English Duke and the wife of a member of Parliament (with whom she’d eloped a couple of years earlier to avoid marrying the unfortunately named Clotworthy Skeffington). Her wit and beauty made her the toast of King George I’s court.
Then she caught smallpox.
She recovered, but with the characteristic pockmarked scars. Early in 1716, she left London behind to accompany her husband to Turkey, where he was the King’s new ambassador to the Ottoman court. In early 1718, she wrote to a friend,
“The small-pox, so fatal, and so general amongst us, is here entirely harmless, by the invention of ingrafting, which is the term they give it. There is a set of old women, who make it their business to perform the operation, every autumn, in the month of September, when the great heat is abated. People send to one another to know if any of their family has a mind to have the small-pox: they make parties for this purpose, and when they are met (commonly fifteen or sixteen together) the old woman comes with a nutshell full of the matter of the best sort of small-pox, and asks what vein you please to have opened. She immediately rips open that you offer to her, with a large needle, (which gives you no more pain than a common scratch) and puts into the vein as much matter as can ly upon the head of her needle, and after that, binds up the little wound with a hollow bit of shell; and in this manner opens four or five veins.”
Soon after, she convinced embassy surgeon Charles Maitland to variolate her five-year-old son, Edward. The procedure went well, and Mary Wortley Montagu was now a woman on a mission:
“I am patriot enough to take pains to bring this useful invention into fashion in England; and I should not fail to write to some of our doctors very particularly about it, if I knew any one of them that I thought had virtue enough to destroy such a considerable branch of their revenue, for the good of mankind. But that distemper is too beneficial to them, not to expose to all their resentment the hardy wight that should undertake to put an end to it. Perhaps, if I live to return, I may, however, have courage to war with them.”
Cotton Mather and the Anti-Vaxxers

The first slaves arriving in Boston in 1683. Image: Library of Congress.
While Lady Montagu learned about inoculation, the practice was also beginning to spread to North America. In Massachusetts, an ageing Puritan minister named Cotton Mather (now best known as the architect of the Salem Witch Trials, which killed 24 people in 1692, mostly women), had a chat about smallpox with an African man named Onesimus, a slave in his Boston household.
“He told me that he had undergone the operation which had given something of the smallpox and would forever preserve him from it,” Mather wrote in a July 1716 letter to physician John Woodward. Onesimus described the inoculation process and showed off the small scar it had left on his arm.
“How does it come to pass, that no more is done to bring this operation, into experiment and fashion in England?” Mather asked Woodward. He was fascinated by the lifesaving potential of inoculation – but he didn’t appreciate the knowledge quite enough to free the man who shared it with him. (Mather did free Onesimus five years later, in 1721, but only after making him raise the money to purchase another slave as a replacement. Nobody ever said Cotton Mather was a nice guy.)
But when a ship from the West Indies sailed into Boston with infected sailors on board in April of 1721, Mather remembered what Onesimus had shared. As a well-known minister in 18th century Massachusetts, Mather had both celebrity and political clout, and he used both to advocate for inoculation. He addressed Boston’s physicians on 6 June 1721, making an earnest case for inoculation as the best way to stop the disease from spreading.
That address stirred up an immediate controversy among Boston doctors and even in Mather’s own congregation. People worried that inoculation would be too dangerous and that it would only spread the disease more quickly. Others argued that it was a “heathen practice” and in defiance of the Puritan view of disease as part of God’s plan for whoever might fall ill.
He managed to convince only one man: a doctor named Zabdiel Boylston (fact: names were at least 48 per cent cooler in the 1700s, with some very obvious exceptions). Boylston launched a variolation campaign, and he sought input on variolation from African slaves around Boston who had experience with the process, though their contributions, like Onesimus’, went mostly unrewarded and remain anonymous to this day.
Things Get Violent

Cotton Mather, about 1700.
Throughout the summer of 1721, Mather published tracts and treatises, gave addresses and sermons, and wrote letters arguing that inoculation was safe, moral, and urgently necessary. But Boston was having none of it. Although people had embraced Mather’s every word when he was calling for the hanging of women in Salem for putting curses on their neighbours, they recoiled at the idea of inoculation. It was a weird time.
In July, he wrote in his diary:
“The Destroyer, being enraged at the proposal of any Thing, that may rescue the lives of our poor People from him, has taken a strange Possession of the People on this Occasion. They rave, they rail, they blaspheme; they talk not only like Ideots but also like Franticks, And not only the Physician who began the Experiment, but I also am an Object of their Fury; their furious Obloquies and Invectives.”
All the while, the infection raged. At its peak, some sources estimate that half of Boston was sick. Boylston inoculated as many people as he could convince, but that wasn’t nearly enough of the population to have any real chance of stopping the spread of the infection. As the epidemic worsened, people blamed Mather and Boylston for its swift, unstoppable spread.
“Towards three a clock in the night, as it grew towards Morning of this Day, some unknown Hands, threw a fired Granado into the Chamber where my kinsman lay, which uses to be my Lodging-Room,” he wrote in his diary on November 14 after a rather eventful night. A relative had travelled to Boston for inoculation and was staying with Mather while he recovered. He almost didn’t make it home.
But Mather and his family were lucky. The firebomb – a heavy iron ball, split into two halves filled with gunpowder and turpentine, according to Mather – hit part of the window casement on the way in and bounced to the floor in a way that just happened to put out the fuse in the process. Because the bomb failed, Mather got to read the message, tied to the fuse with string: “COTTON MATHER, You Dog, Dam you; I’ll inoculate you with this, with a Pox to you.”
To make his case for variolation, Mather published data on the fatality rate for inoculation – about 2 per cent – and for actual smallpox infection – about 14 per cent in the Boston outbreak. It was the first documented use of comparative data in medicine, and it eventually helped persuade people to accept inoculation.
Meanwhile, Back in England

Lady Mary Wortley Montagu.
That same year, Lady Montagu insisted that Charles Maitland inoculate her four-year-old daughter in a demonstration for the royal physicians. It worked, and in August, the King gave Maitland permission to conduct a trial of the technique on prisoners in London’s Newgate Prison. Six men volunteered on the promise of the King’s pardon for the survivors.
When all six prisoners survived and later proved to be immune to smallpox, Maitland moved on to testing his inoculation on orphaned children, who were slightly less expendable than convicted criminals. But only slightly.
The plucky orphans also survived, so Maitland moved on to inoculating princesses (skipping several rungs on the expendability ladder). In April of 1722, he inoculated the daughters of the Princess of Wales. After that, inoculation started to catch on in England, though it took another few decades to become widely accepted in the rest of Europe. According to Voltaire in 1774,
“It is inadvertently affirmed in the Christian countries of Europe that the English are fools and madmen. Fools, because they give their children the small-pox to prevent their catching it; and madmen, because they wantonly communicate a certain and dreadful distemper to their children, merely to prevent an uncertain evil. The English, on the other side, call the rest of the Europeans cowardly and unnatural. Cowardly, because they are afraid of putting their children to a little pain; unnatural, because they expose them to die one time or other of the small-pox.”
Variolation had actually been banned in France for five years, from 1762 to 1767, after it caught the blame for an outbreak. But in 1774, when King Louis XV died of the disease after two weeks of illness, along with 10 other members of his court, his son – the newly crowned King Louis XVI — boldly decided to have himself and his two younger brothers variolated (the guillotine, rather than smallpox, finished off Louis XVI).
And eventually, inoculation did catch on in Europe, partly thanks to the data published by Mather and others, and partly thanks to Lady Montagu’s trendsetting advocacy in England. It was the best defence against smallpox until 1840, when England banned variolation in favour of a new preventative: vaccination.
How Vaccination Went Viral

A milkmaid and cows, sometime between 1790 and 1843. Image: Dordrechts Museum via Wikimedia Commons.
Thirty-five years later, in 1757, a young boy named Edward Jenner received an inoculation against smallpox. Eventually, he also received most of the credit for developing the first smallpox vaccination: a way to give people immunity smallpox without exposing them to the live smallpox virus.
Cows’ udders sometimes become infected with a virus that causes small pustules, similar to smallpox but less severe. The two viruses are closely related – so closely that the human immune system has trouble telling them apart. So exposure to one will help you develop immunity against the other. In the 1700s, most people in Gloucestershire and the surrounding counties knew, or at least suspected, that exposure to cowpox kept milkmaids from catching its deadlier cousin, smallpox – just as people all around the world knew that variolation worked for years before Montagu, Maitland, Mather, and Boylston. That’s how Jenner heard about the connection between cowpox and immunity to smallpox; he spent the early days of his medical career in a dairy community.
In May of 1796, he tested cowpox inoculation on the nearest available child – as one does, presumably. Eight-year-old James Phipps suffered from a mild fever and aches for about nine days, and then felt better.
So of course Jenner inoculated him with smallpox a couple of months later. Phipps didn’t get sick. The cowpox had given him immunity to smallpox.
Jenner self-published his results in 1798, after rejection by the Royal Society. He called the new technique “vaccination,” from the Latin word vaccinia for cowpox. By inoculating people with cowpox, it was possible to protect them from smallpox, without actually exposing them to the deadly
Today, the word “vaccine” is a generic term for any substance that causes the body to develop immunity to a disease. Usually, vaccines are made from dead or weakened forms of the virus being vaccinated against. Modern vaccines use viruses, or antigens from viruses, grown in cultures in a laboratory – not an actual gob of someone else’s infected pus. We’ve come a long way.
Whose Discovery Was It?

Benjamin Jesty in 1805. Source: Jesty.org via Wikimedia Commons
Today Edward Jenner is known as the father of vaccination – but he wasn’t the first to inoculate with cowpox. In fact, the first person to vaccinate with cowpox wasn’t even a doctor.
In 1791, a German teacher named Peter Plett inoculated three children with cowpox; like Jenner, he had learned about the connection from milkmaids (who probably deserve most of the credit in the long run). When he reported his results to professors of medicine at the nearby University of Kiel, they basically ignored him, so Plett resumed his teaching career. He got a little recognition in the early 1800s, but barely a footnote compared to the accolades Jenner eventually received.
But even Plett wasn’t the first. A Dorset cattle farmer named Benjamin Jesty inoculated his wife and two sons with cowpox (and one of his wife’s knitting needles) in 1794 to protect them from a nearby smallpox outbreak. That claim is carved in stone – literally. The epitaph on Jesty’s tombstone calls him “an upright honest Man; particularly noted for having been the first Person (known) that introduced the Cow Pox by Inoculation, and who from his great strength of mind made the Experiment from the (Cow) on his Wife and two Sons in the Year 1774.”
Ultimately, of course, it’s probably the milkmaids and dairy farmers of rural Europe who deserve the credit for discovering the smallpox vaccine.
So why does Jenner get all the credit? Although the link between cowpox and smallpox immunity was pretty well known in dairy farming areas, it was still a new idea outside those areas. Jenner might not have been the first person to figure out the connection, or even to apply that knowledge to inoculation, but he did bring it to the attention of the scientific community and convince them to accept it.
In the words of Victorian statistician and scientist Francis Galton, “In science, credit goes to the man convinces the world, not the man to whom the idea first occurs.”