Nearly a century after scientists dug up penicillin, researchers are turning once more to the soil for new pharmaceuticals. But this time, they have tiny, powerful technologies on their side. Here’s how scientists are unlocking the secrets of soil microbes and discovering the next generation of medicine.
Soil is the most biodiverse habitat on the planet, containing upwards of 10 billion bacteria and fungi in a single gram. It’s also a vicious battlefield, where microbes are engaged in an endless chemical arms race, exuding all sorts of antibiotics and toxins as they compete for resources. Indeed, the very first group of antibiotics every discovered, penicillin, comes from a fungal decomposer found in forest soils across the world. In the mid 20th century, many other well-known antibiotics, including widespread and excessive use of antibiotics in animal agriculture and human medicine, the incidence of drug resistant
infections has skyrocketed. Health officials are making dire predictions of a post-antibiotic future, and the realities such a future would hold are harrowing.
The message is resoundingly clear: We need to discover new dugs, and fast.
From Petri Dishes to Meta-Genomes
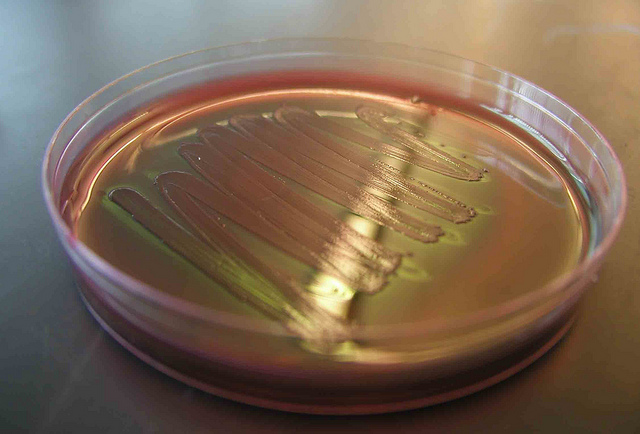
Image: Anthony D’Onofrio
In the old days, if you wanted to study a microbe, that meant getting it to grow in the lab. But finding the growth conditions that work for most bugs has proven extraordinarily challenging. To this day, we’ve only managed to culture roughly one per cent of the soil microbes we think are out there. For decades, the identity of “unseen majority” was a complete mystery.
But in the last twenty years, new, high-throughput technologies have brought microbiology out of the dark ages. Researchers can now take a sample of dirt, water, air or sludge, suck the DNA out of it and decode its entire genetic library. We can ID every microbe in a spoonful of dirt without growing a thing. The field of metagenomics
has revolutionised our view of the world, showing us that we’re really just a small part of a vast microbial ecosystem, or microbiome.
But as Sarah Zhang pointed out recently, we’re still like 19th century Darwinian explorers when it comes to microbiomes: We’re in the phase of cataloging life. This is an important endeavour, but it also has inherent limitations.
Imagine you wanted to learn about the people of New York City, and you did so by taking a skin sample from every resident, and sequencing their genomes. You’d learn a lot about ancestry, genetic relationships, perhaps even susceptibility to disease. But you’d learn next to nothing about what the Big Apple’s residents can actually do. How many doctors and policemen are there? How many people are bilingual? Who’s a proficient programmer and who can electrically wire a house? To learn any of that, you’d need to actually observe human beings and see what they’re capable of.
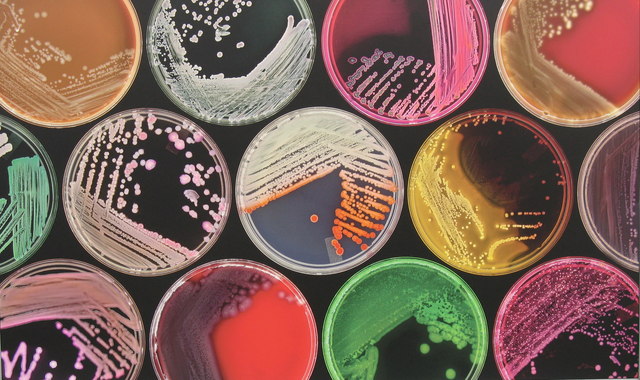
Image: M.J. Richardson
By the same token, researchers can use metagenomics to discover what microbes exist in nature, but to learn what our microbial subjects are actually doing, we need to see them in action.
“There is much that’s still not explainable by looking at the genome of an organism,” Slava Epstein, a professor of biology at Northeastern University, told me. “At the end of the day, the properties of an organism, such as the antibiotics it can produce, are still much easier to discover if you can culture the organism.”
Which brings us to teixobactin, a promising new class of antibiotic whose discovery was based on iChip, a technology that blends old-school culturing with new-school approaches aimed at tapping the unseen majority as efficiently as possible.
A Game Changing Technology
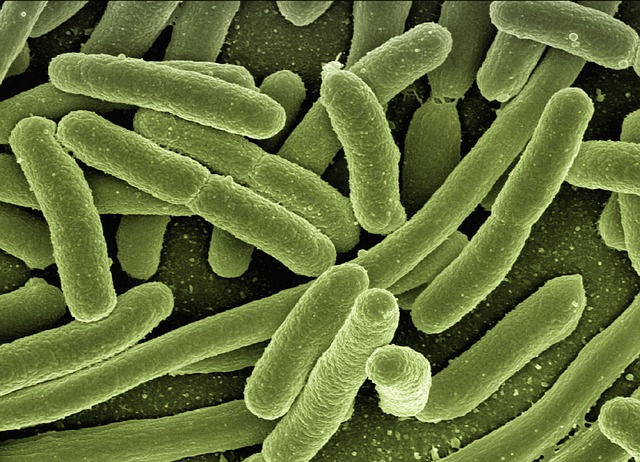
When teixobactin was announced back in January, it was hailed as a “game-changer” in the fight against antibiotic resistance. And for good reason: It’s the first new class of antibiotics we’ve discovered in nearly thirty years, and so far, it’s killed every pathogen we’ve thrown at it, including several highly drug-resistant strains of staph. Unlike most antibiotics, which target critical bacterial proteins, this drug attacks the lipid molecules bacteria use to build new new cell walls. Vanomycin, another antibiotic that targets cell wall precursors, worked for over 40 years before bugs started to develop resistance.
Image: Pixabay
Still, there are important realities we need to face. For one, teixobactin is still in pre-clinical development, and there’s no guarantee that the drug will make it to market. But even if it does, teixobactin is not going to be the silver bullet that solves our antibiotic crisis. Because if there’s one thing microbes have shown us time and again, it’s that they’re capable of developing resistance to just about everything — from antibiotics to powerful acids to radioactive waste. Like other antibiotics, teixobactin needs to be managed responsibly to extend its lifespan as much as possible. Even so, some bacteria will eventually evolve resistance.
What’s more game-changing than anything about this particular drug is how we found it. Teixobactin was isolated from a previously uncultured soil bacterium, using a clever little gadget called iChip, which is now licensed to the company NovoBiotic Pharmaceuticals, founded by Epstein in the early 2000s.

iChip. Photo courtesy of Slava Epstein
The principle behind iChip is quite simple: Most soil microbes can’t be grown in the lab, so instead, let’s grow them where they grow best — the dirt.
“For one hundred and fifty years, all microbiological cultivation was, in essence, guesswork,” Epstein told me. “But we know that nature provides the essentials these organisms need. If that’s the case, then why on Earth do we try to cultivate them in the lab?”
Epstein has been working for over a decade to bring microbial cultivation to the field, and now, his company has designed a clever way of doing so. iChip is a small grid composed of hundreds of miniature growth chambers. Soil is diluted in water, mixed with agar, and poured into the chip. The dilution ensures that each “chamber” contains only a single bacterium to start. The chip is then dunked in a beaker of soil and the bacteria are allowed to grow. They stay put because of the agar, but are otherwise exposed to all the nutrients and growth factors they need. Once each “seed bacteria” has multiplied, researchers can screen the chip for interesting products, including antibiotics.
So far, iChip is off to an exciting start. It’s collected roughly 10 thousand strains of uncultured soil bugs and uncovered a handful of new antibiotics, including teixobactin. And this is just the beginning — remember, the majority of antibiotics we’ve discovered and developed so far come from a mere 1 per cent of soil bacteria. In the remaining 99 per cent, we expect to find hundreds to thousands more, as well as anti-inflammatories, anti-virals, anti-cancer agents, and immunosuppressives. A veritable treasure trove of drugs.
What’s more, iChip’s early success is motivating new initiatives to unlock the medical potential of soil microbes. These include the citizen science project Drugs from Dirt, which seeks to map the genetic diversity of soils worldwide using metagenomics. Such a map could allow researchers to identify “hotspots” for medically valuable bacteria, which could be further investigated tools like iChip.
“There is a helpful dichotomy here, between metagenomics and new cultivation tools,” said Epstein. “Both want to achieve the very same thing: accessing the potential of those microorganisms in soil that cannot be cultured in the lab.”
Genomics tools and cultivation might be synergistic in other ways, too. For instance, once an antibiotic-producing bug has been identified, researchers might be interested in knowing its entire genome, to see what else it’s capable of.
“Right now, we’re focused on cultivation, but that’s not to say we’re not interested in knowing the genomes the strains we cultivate,” Epstein told me. “That would tell us not only what we see them producing, but what they can potentially produce. In the future, perhaps we could find a way to utilise those hidden powers.”
With a plethora of new, high-throughput screening tools at their disposal, researchers like Epstein are optimistic that a return to the glory days of discovering drugs in the dirt is upon us. Let’s hope so, because the only way we’re going to beat bacteria at the drug resistance game is to uncover powerful new weapons faster than they can evolve defence.
So, next time you find yourself a little muddy after walking around outside, take a moment to appreciate that glob of dirt caked to the bottom of your boot. Buried within it might just a bug that will save millions of lives.
Top image via Shutterstock
