Upon his return from six weeks volunteering with the King’s Sierra Leone Partnership at a number of Ebola isolation facilities in Freetown, Tom Boyles considers the endgame of the Ebola epidemic.
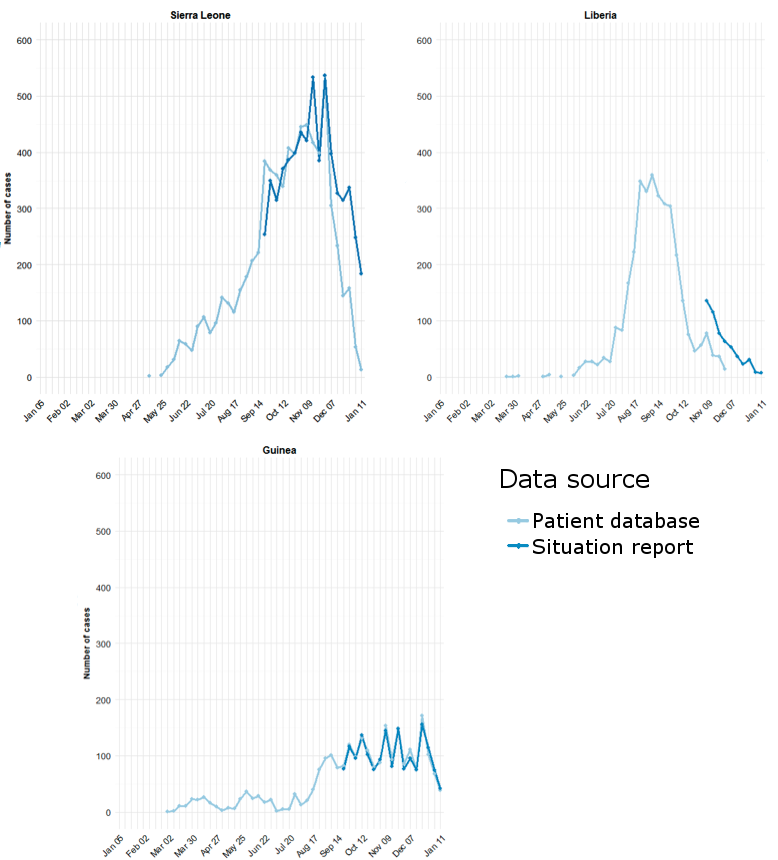
There are encouraging signs of an overall reduction in confirmed cases of Ebola in west Africa. The graphs below show the epidemic curves for Sierra Leone, Liberia and Guinea as of 14 January 2015 and current data can be found here. Clearly there has been a dramatic reduction in cases in the first 2 countries although in Guinea the epidemic seems to be grumbling on at a lower level. These graphs may signal the beginning of the endgame but one of the important questions at this point is “How will the Ebola epidemic end?” and no-one is quite sure. Having recently worked on the Ebola response in Sierra Leone my suspicion is that when the end finally approaches we will have a significant ‘last mile problem’; what some others have described as a long and bumpy tail to the epidemic. We will need to ensure that the very last patient either dies or survives without infecting anyone else and this will be easier said than done.
From the beginning it has been vital to avoid losing focus on other interventions such as childhood vaccination programme so that the Ebola crisis is not followed by a measles epidemic, for example. In order to keep healthcare facilities open the model in Freetown has been to put screening services and small isolation units at each one. The over-riding aim is to protect the facility staff from Ebola so they can continue with their everyday work. Patients who screen positive are isolated and tested for Ebola; positive cases are then transferred to dedicated treatment centres and negative cases either discharged home or to the healthcare facility if they need ongoing care. This model has been largely successful in protecting staff at facilities and allowing some normal services to continue.
The screening algorithm is highly sensitive to prevent any positive cases slipping through the net and putting healthcare workers at risk, as a result there will always be a proportion of patients who do not have Ebola but screen positive. While transmission has remained intense this proportion has remained relatively low (around 30%) and it has been easy for staff to remain motivated. Questions remain about what will happen when case numbers drop to very low levels and an ever increasing proportion of those screening positive turn out not to have Ebola; at that point there is a grave danger that complacency will set in. A small facility might go several weeks without seeing a positive case and staff might be tempted to decide that a patient with fever, headache and malaise actually has malaria and to treat them accordingly rather than isolating them. It will only take a couple of errors of this nature to send infectious patients back into the community or to infect a new batch of healthcare workers and the cycle of fear and infection will restart.
It is not only healthcare facilities that need to guard against complacency. A similar problem could occur in a village that has not seen a case for a few weeks or months and begins to feel safe. The cultural drive to clean corpses and sleep next to them for several nights before burial is strong and is one of the major drivers of transmission. It is not unheard of for a single unsafe funeral to account for dozens of new infections so it only takes one such event to re-ignite the transmission cycle. It will be vital to keep up the message that any corpse might be highly infectious and must be buried safely.
Sierra Leoneans are already weary from this battle. Schools and universities remain closed and there is an ongoing partial lockdown in Freetown. They want nothing more than to see the back of the epidemic. As it drags we will need to re-double our efforts to avoid complacency and a re-ignition of the transmission cycle. In this epidemic it could well be the last mile that is the longest.
This article first appeared on PLoS Blogs and is republished under Creative Commons licence. Dr Tom Boyles is a consultant in Infectious Diseases and HIV Medicine at the University of Cape Town. He has written about his time in a blog.