When Kaiba Gionfriddo was born, his parents never expected to have to look on, helpless, as his windpipe collapsed daily and stopped him from breathing. They were desperate — so when a team of researchers suggested that a 3D printer could help, they leapt at the chance.
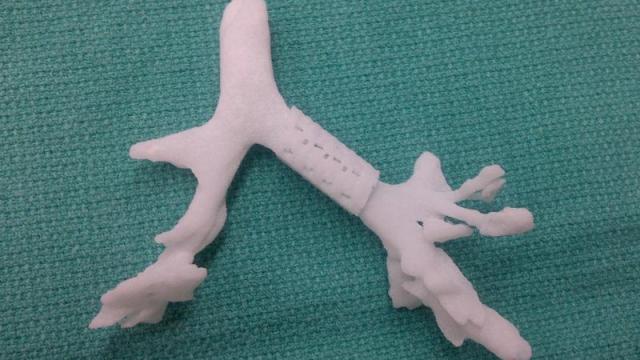
So a team from the University of Michigan set about using high-resolution imaging to study Kaiba’s trachea and bronchus, and then got busy with some computer-aided design. Using data from CT scans, they were able to create accurate 3D models of his delicate little airways — weakened by a condition called tracheobronchomalacia — and develop a splint that could be used to help support them. The research is published in the New England Journal of Medicine.
Once it was designed, the splint was 3D-printed using a biopolymer called polycaprolactone, which, over the course of two to three years, is completely reabsorbed by the body. Last year, the splint was sewn around Kaiba’s airway to expand the bronchus, giving it a stiff structure for support which it can grow around.
Just 21 days after the operation Kaiba was taken off ventilator support — and he hasn’t needed it since. Dr Scott Hollister, the professor of biomedical engineering behind the 3D-printed implant, explains how delighted the team is:
“The material we used is a nice choice for this. It takes about two to three years for the trachea to remodel and grow into a healthy state, and that’s about how long this material will take to dissolve into the body. Kaiba’s case is definitely the highlight of my career so far. To actually build something that a surgeon can use to save a person’s life? It’s a tremendous feeling.”
Of course, it’s not the first time 3D printing has had a positive effect in medicine, but it’s an amazing result nonetheless — and it also offers huge hope for the 1 in 22,000 babies who suffer severe cases of tracheomalacia. We’re glad Kaiba — and his parents — can now breathe easy. [NEJM via Science Daily via Y Combinator]