Monkeypox is the latest emerging germ to alarm public health experts, with over 4,000 reported cases globally this year. While this viral illness may not be as fast-spreading as COVID-19, it’s threatening to shift from a zoonotic disease, rarely spread from rodents, to something that regularly jumps between humans from here on out, perhaps predominantly as a sexually transmitted infection.
Monkeypox’s most distinctive symptoms are the contagious bumpy rashes that form a week or two after exposure, which can last for up to a month. But unfortunately, rashes and odd skin growths can occur for any number of reasons. So for those of us who might get understandably paranoid about seeing new bumps show up on our skin these days, here’s a rundown of eight rashy conditions that aren’t monkeypox.
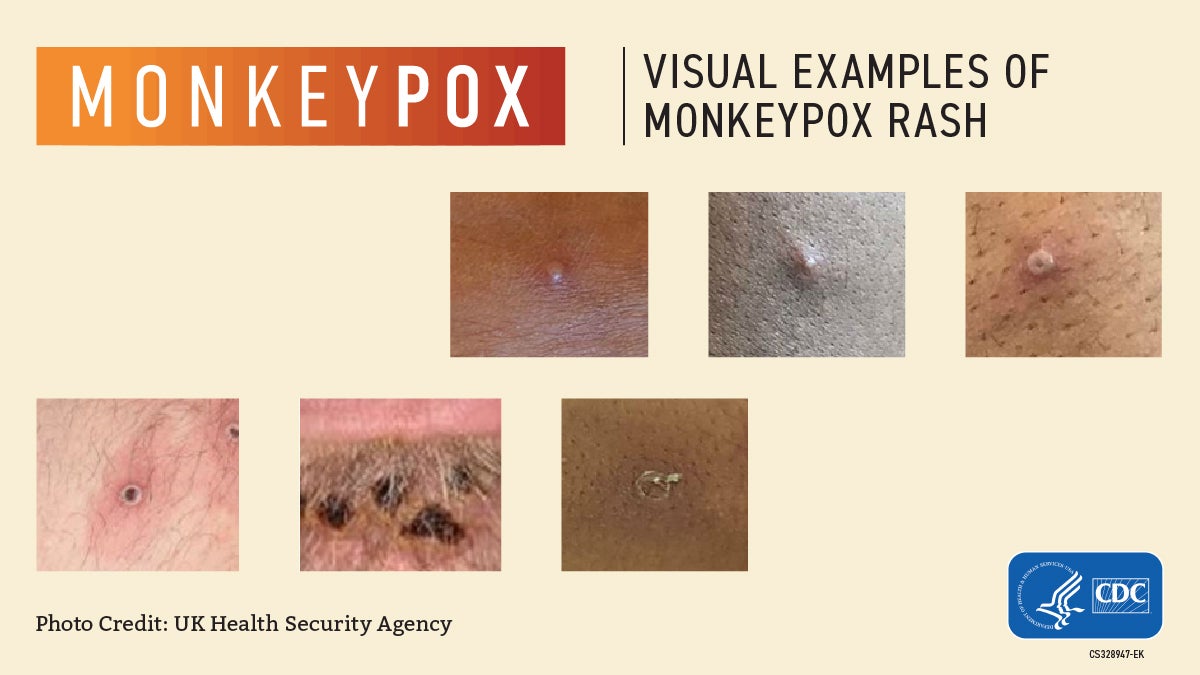
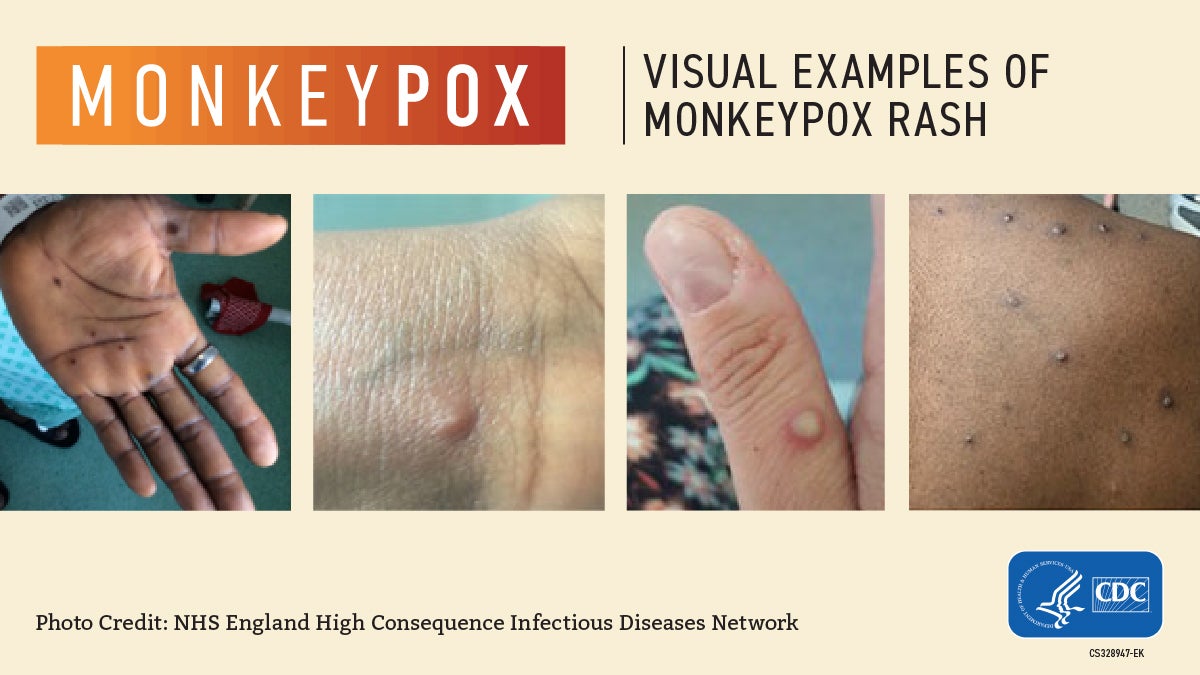
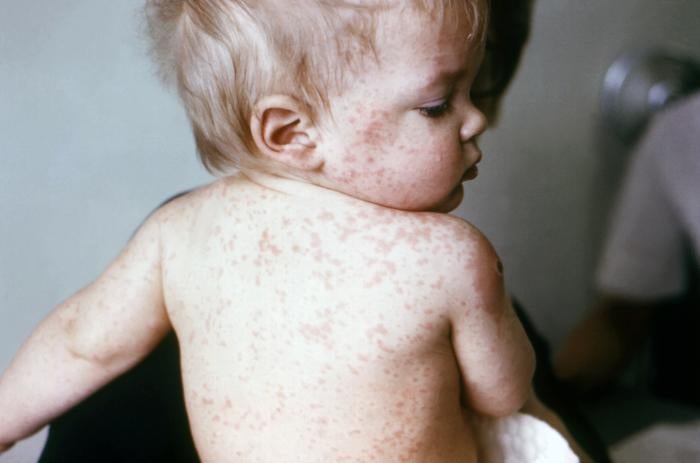
And for reference, here’s what actual monkeypox looks like:
Scabies
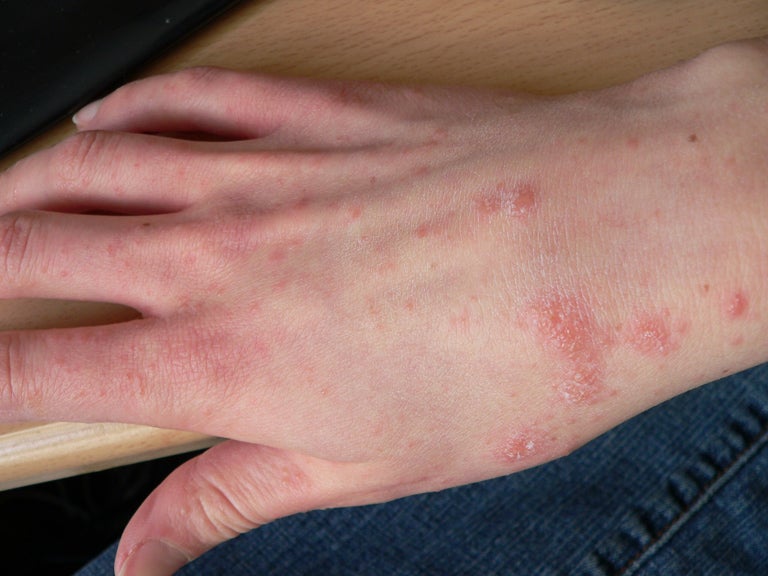
Why it happens: Scabies is caused by an infestation of the arachnid Sarcoptes scabiei, or the human itch mite. Its symptoms are a result of the body’s allergic response to the mites burrowing and travelling under our skin, as well as the later laying of their eggs. The mites are spread through close prolonged contact, including during sex.
Symptoms and treatments: Scabies is characterised by an intense itch, along with pimple-like rashes, at the site of infestation, which is usually along our arms or feet. People with weaker immune systems tend to develop more intense infestations and crusty-looking rashes. The mites can be treated with topical or oral antiparasitics, but people can get them again in the future. The first time someone is affected, it can take up to eight weeks for symptoms to appear, but as little a day for subsequent encounters.
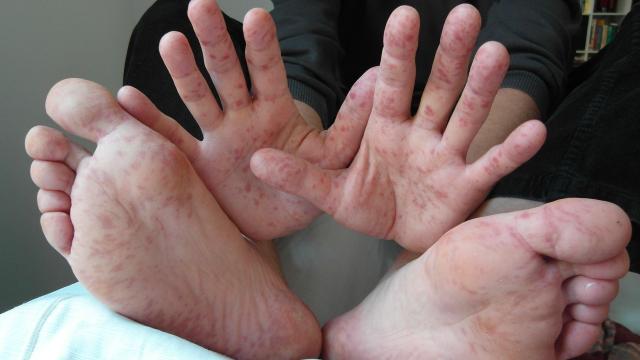
Hand, foot, and mouth disease
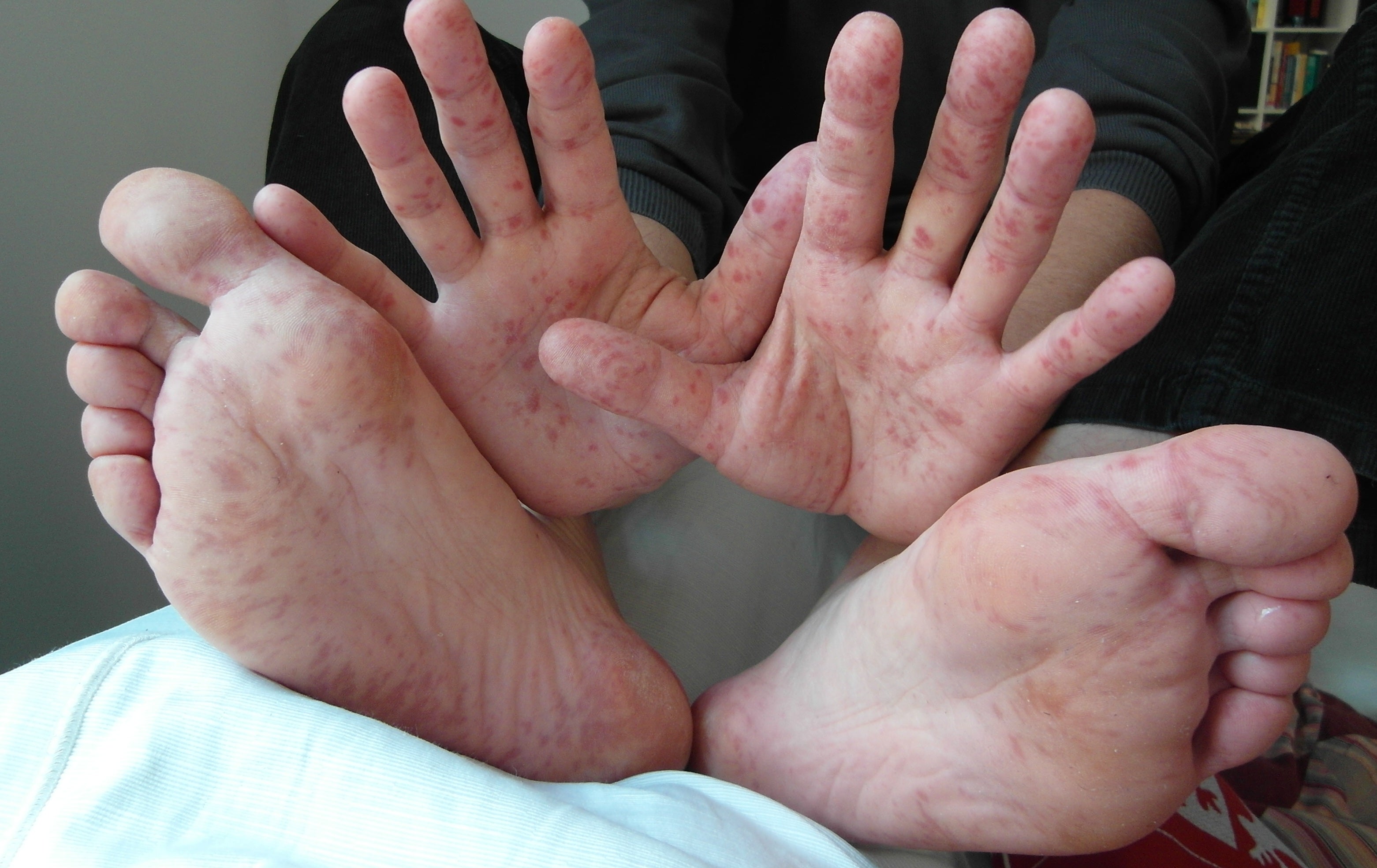
Why it happens: Hand, foot, and mouth disease is caused by infection from a group of related viruses, though most cases in AU are caused by the Coxsackievirus A16. The infection typically affects children under five.
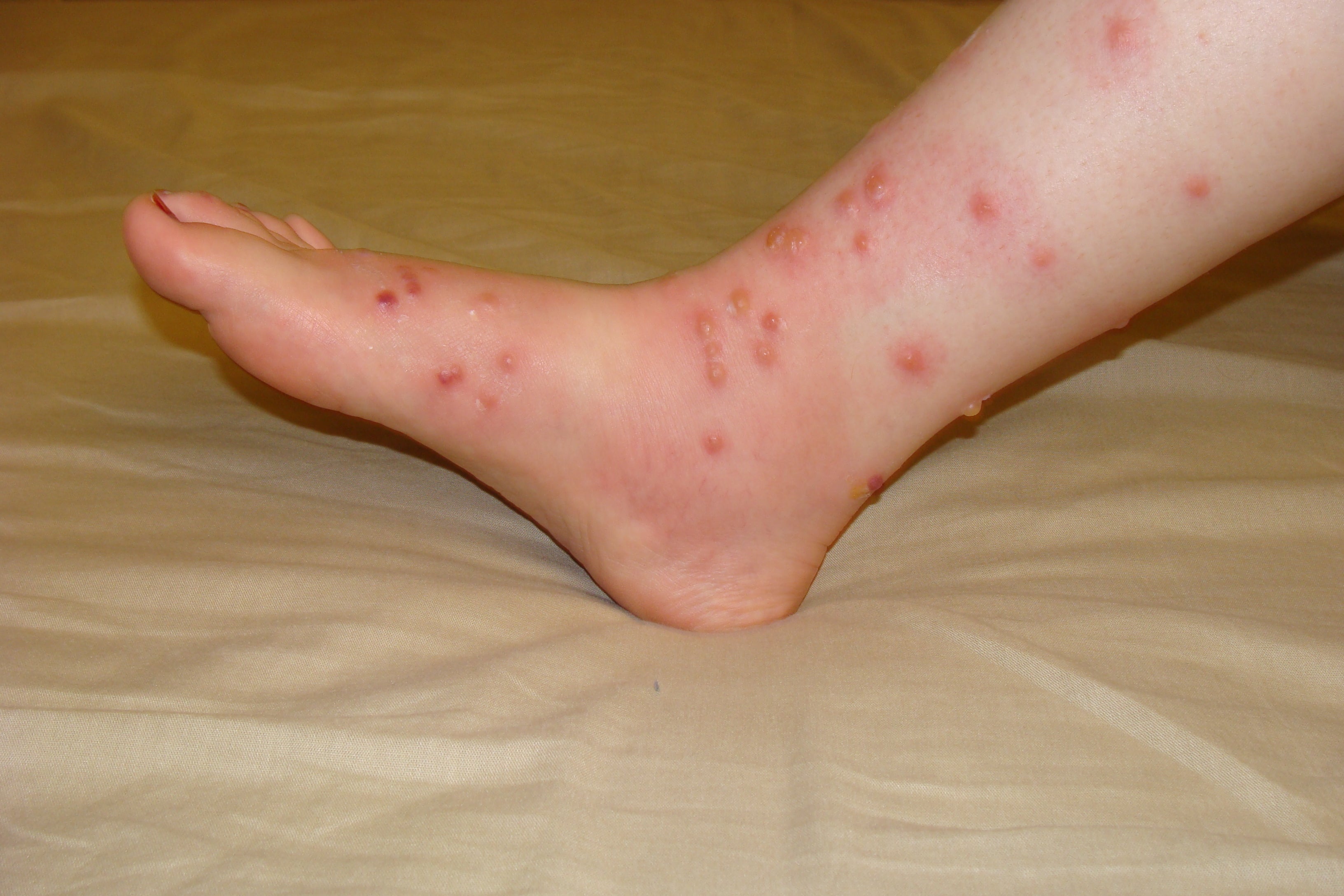
Symptoms and treatments: The condition presents as flat or slightly raised red bumps along a person’s hands, feet, and mouth. These bumps can sometimes develop into fluid-filled blisters that further spread the very contagious infection through direct contact. There’s no specific treatment, but cases are usually very mild, and symptoms often resolve on their own within a week or so.
Ringworm
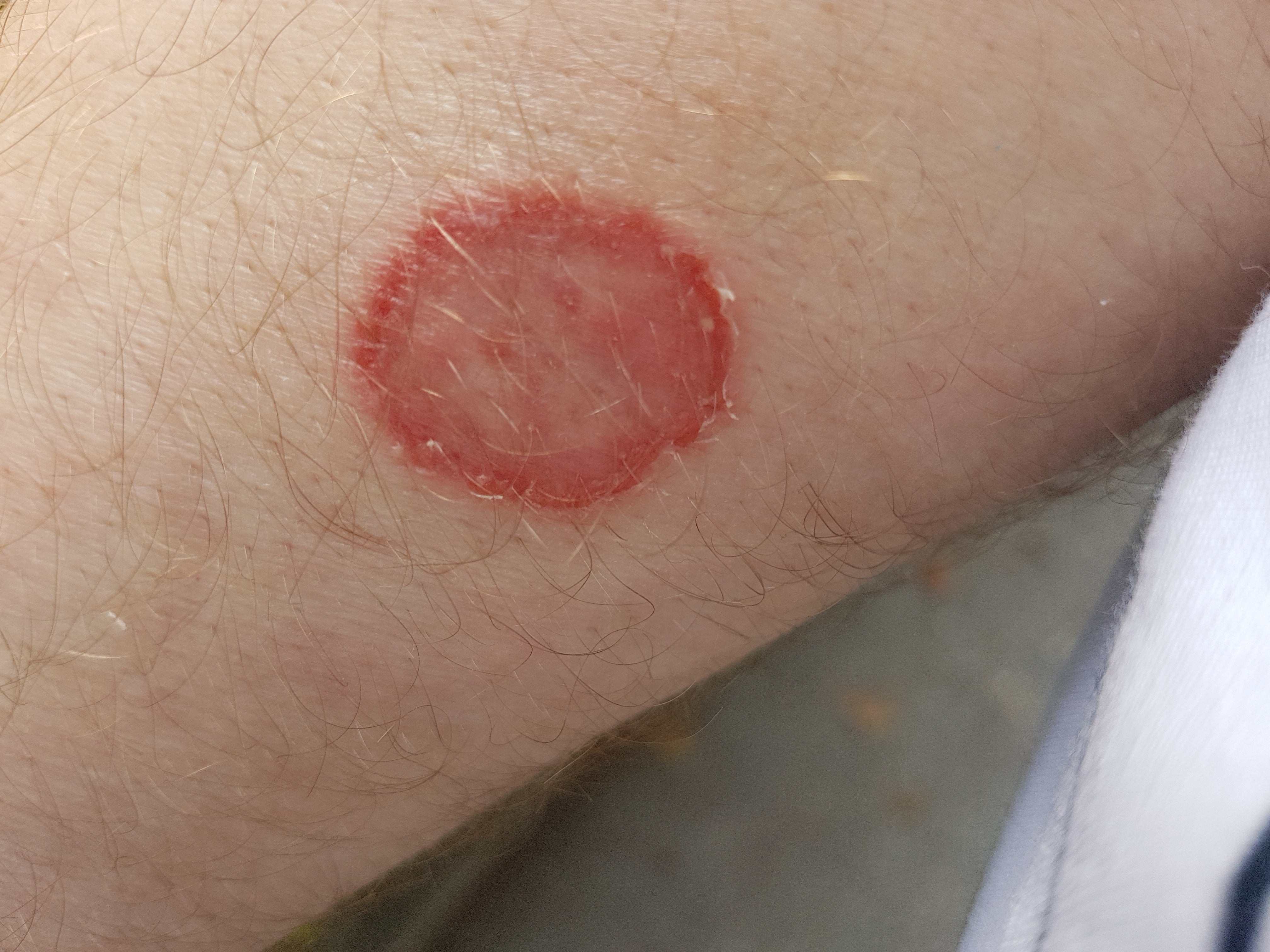
Why it happens: Ringworm (tinea) isn’t actually caused by a worm at all. It’s instead a broad term for common fungal skin infections that cause similar symptoms. More than three dozen fungal species can cause ringworm. Skin conditions like athlete’s foot (the feet) and jock itch (around the genitals) refer to such infections found on specific parts of the body.
Symptoms and treatments: The infection triggers a tell-tale circular rash, along with itchy, red, and sometimes cracked skin. If found in the scalp or other hairy places, it can also cause hair loss. Most infections can be treated easily enough with a two-to-four-week course of over-the-counter antifungal creams, lotions, or powders. But scalp infections usually require prescription oral antifungals. People with ringworm should not use steroid creams, which can help treat other rashy conditions, since these can suppress the immune system and make the infection worse.
Shingles
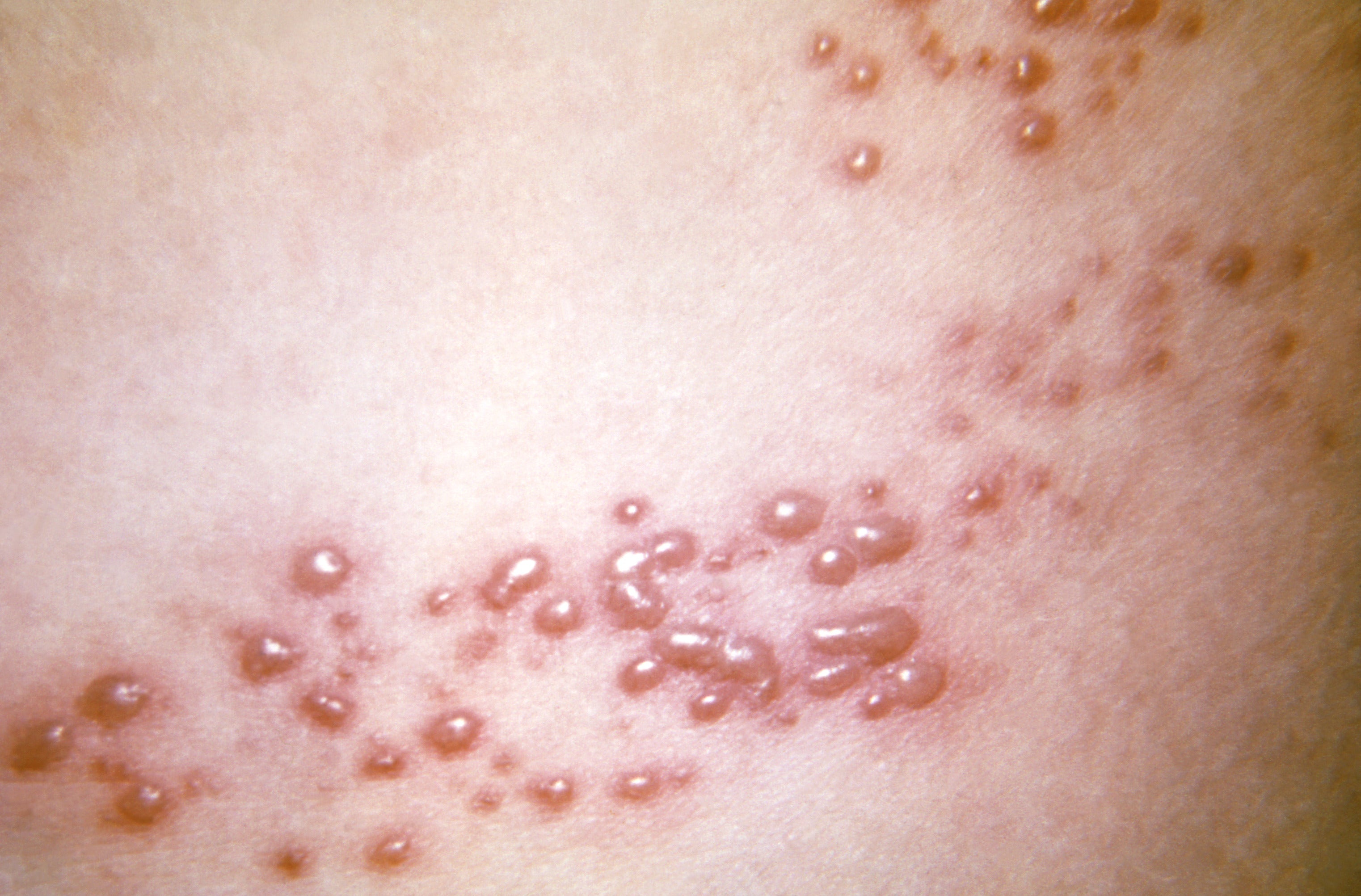
Why it happens: Shingles is caused by the same virus behind chickenpox, herpes zoster. Following the initial infection, usually in childhood, the virus migrates to the nervous system and can lay dormant for decades before reemerging to trigger shingles.
Symptoms and treatments: Common symptoms at first include excruciating pain and numbness along one side of the body or face, followed by rashes and fluid-filled blisters. It takes weeks for these rashes to heal and scab over, and some sufferers can be left with lingering nerve pain where the rashes formed. There is no specific treatment for shingles, but people vaccinated against chickenpox as children are much less likely to develop it, while older adults who caught chickenpox naturally can get a separate vaccine for shingles that greatly reduces their risk of having it as well.
Hives
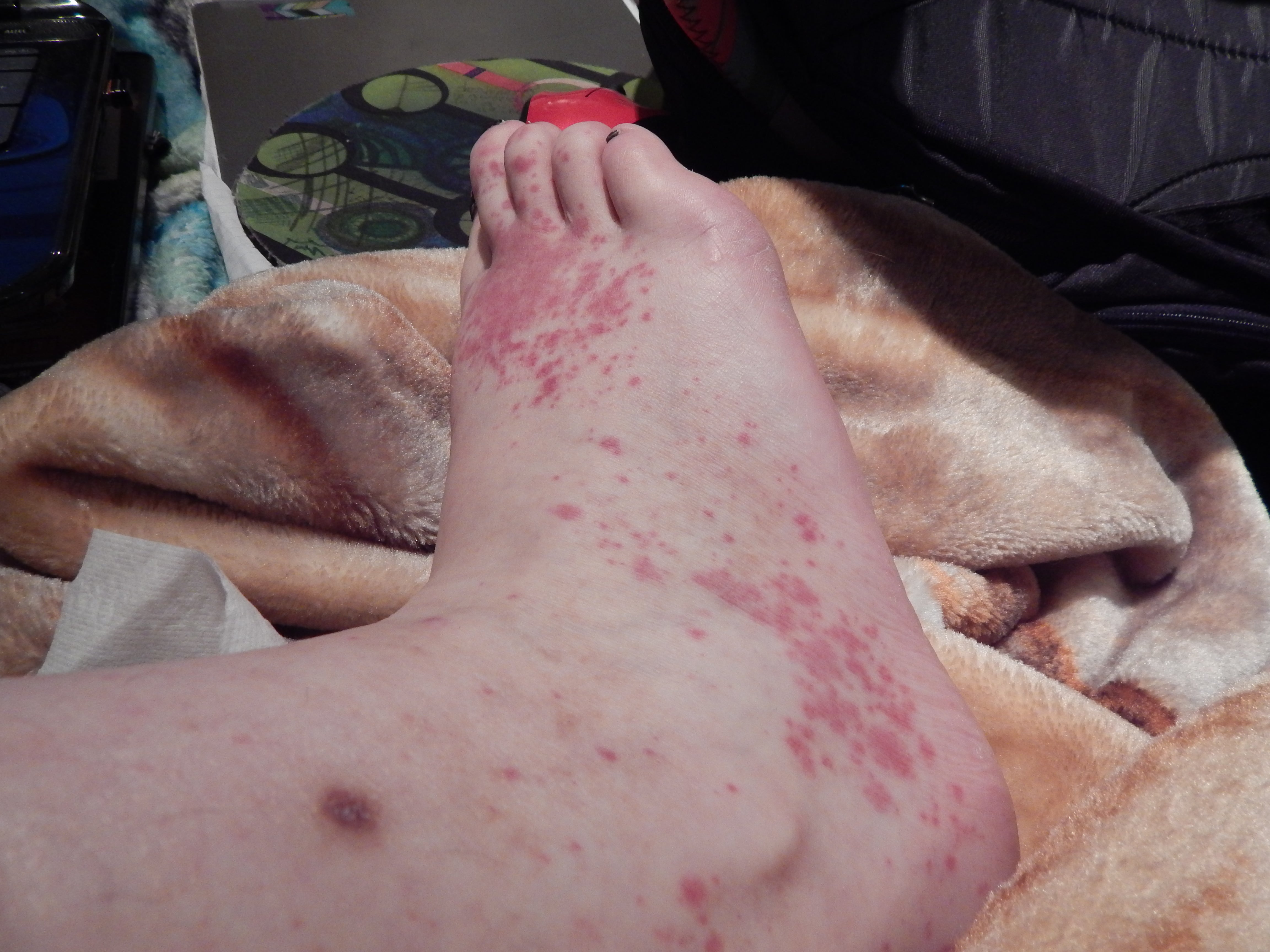
Why it happens: Hives, also known as urticaria, are caused by an immediate allergic reaction to substances like insect stings, pet dander, or certain foods, though an exact trigger may not always be easy to identify.
Symptoms and treatments: Itchy, red welts that appear along the limbs, chest or face soon after exposure to a trigger. Though hives themselves aren’t especially dangerous, they can sometimes accompany a more severe and life-threatening allergic reaction called anaphylaxis. Acute hives tend to fade away on their own within hours or days, but some people can have chronic episodes that can last longer than six weeks. Antihistamines are commonly used to treat or prevent hives, and steroids may be used for more serious or chronic cases.
Measles
Why it happens: Measles is caused by its namesake virus (Measles morbillivirus). It’s very contagious among people with no preexisting immunity to it, such as the unvaccinated and very young children.
Symptoms and treatments: The infection initially presents a flu-like illness, followed by flat red spots and sometimes small raised bumps that start at the face and travel all throughout the body. The illness is usually mild, though younger children are more likely to develop severe, life-threatening complications like pneumonia and brain swelling. An infection can also reset a person’s immunity to other diseases. There are no specific treatments for measles, but there is a highly effective childhood vaccine against it. Unfortunately, declining global vaccination rates have led to its resurgence in some parts of the world.
Poison ivy rashes
Why it happens: Poison ivy rashes are caused by a specific type of allergic reaction known as contact dermatitis (this reaction is different from the one that causes hives). The actual trigger is the oily coating on the plant’s leaves, stems, or roots, known as urushiol, which can even be spread through contaminated clothing.
Symptoms and treatments: Dry, flaky skin along with red, itchy rashes that appear at the site of exposure and a burning sensation. These rashes can sometimes swell up and turn into oozing blisters. Unlike hives, this reaction can take hours or even days to show up after an exposure. If you know you’re allergic to poison ivy, washing the oil off as soon as possible can reduce symptoms, while steroid creams may mitigate swelling. A typical poison ivy rash will clear up on its own within two weeks, but people who have inhaled smoke from burning the plant can develop severe breathing problems that require urgent medical attention.
Warts
Why it happens: Warts are caused by infections with certain types of the human papillomavirus. The types of HPV that cause warts are not the types that can cause cancer.
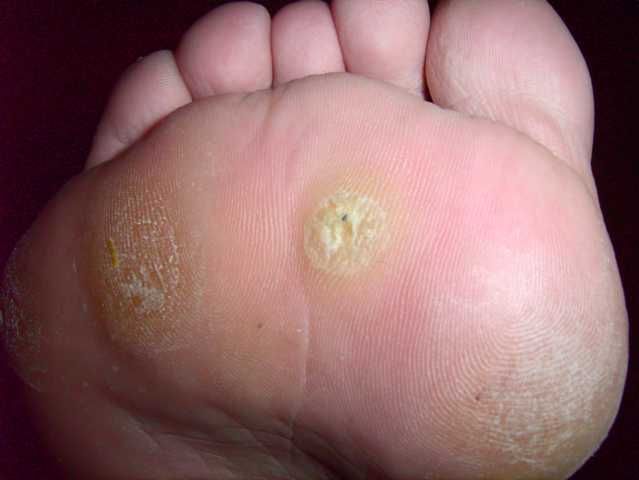
Symptoms and treatments: The appearance of warts can differ depending on where they show up, but they’re typically small, rough-feeling growths on the skin. They most often appear on our hands, but some HPV types can cause warts on our genitals, face, or feet. While the warts themselves are usually harmless, they are contagious and can sometimes be painful. They often go away on their own, but over-the-counter treatments like topical salicylic acid can speed up the process. Recurring or long-lasting warts can be surgically removed or cauterized. Warts are benign, but similar-looking growths that grow in size or shape may be a sign of cancer.