Expert human pathologists typically require around 30 minutes to diagnose brain tumours from tissue samples extracted during surgery. A new artificially intelligent system can do it in less than 150 seconds—and it does so more accurately than its human counterparts.
New research published today in Nature Medicine describes a novel diagnostic technique that leverages the power of artificial intelligence with an advanced optical imaging technique. The system can perform rapid and accurate diagnoses of brain tumours in practically real time, while the patient is still on the operating table. In tests, the AI made diagnoses that were slightly more accurate than those made by human pathologists and in a fraction of the time. Excitingly, the new system could be used in settings where expert neurologists aren’t available, and it holds promise as a technique that could diagnose other forms of cancer as well.
During cancer surgery, it’s not uncommon for surgeons to extract some potentially problematic tissue for lab analysis. These intraoperative biopsies allow for more accurate diagnoses and to help the medical team devise next steps, such as scheduling a subsequent surgery to remove the tumour.
According to the new study, around 1.1 million brain samples are biopsied in the United States each year—all of them meticulously scrutinised by a trained neuropathologist. This process, as the authors wrote in the paper, is “time, resource, and labour intensive.”
Indeed, these diagnoses involve over a dozen steps, including transporting the tissue from the operating room to the lab and temporarily placing it in a cryogenically frozen state, thawing and dehydrating the sample, clearing it with xylene, and mounting it in a microscope for analysis—not to mention all the steps required by the pathologist to perform their evaluation of the tissue. To compound the problem, there’s currently a shortage of neuropathologists in the United States, and “further shortages are expected given the 42% vacancy rate in neuropathology fellowships,” according to the study.
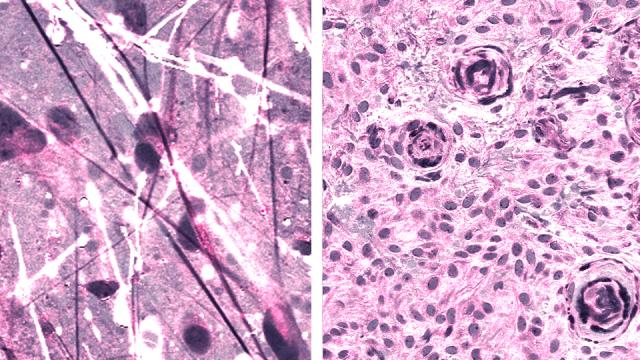
Looking to streamline this process, New York University neuroscientist Daniel Orringer and his colleagues developed a diagnostic technique that combined a powerful new optical imaging technique, called stimulated Raman histology (SRH), with an artificially intelligent deep neural network. SRH uses scattered laser light to illuminate features not normally seen in standard imaging techniques. During surgery, images acquired through SRH are evaluated by the AI algorithm, which needs less than 150 seconds to make its assessment, compared to the 20 to 30 minutes required by human neuropathologists. The authors “demonstrated how combining SRH with deep learning can be employed to rapidly predict intraoperative brain tumour diagnosis,” according to the paper.
Fascinatingly, the AI is also capable of detecting features in the biopsies not visible to the human eye.
“As surgeons, we’re limited to acting on what we can see; this technology allows us to see what would otherwise be invisible, to improve speed and accuracy in the [operating room], and reduce the risk of misdiagnosis,” Orringer, the senior author of the paper, said in a press statement. “With this imaging technology, cancer operations are safer and more effective than ever before.”
To create the deep neural network, the scientists trained the system on 2.5 million images taken from 415 patients. By the end of the training, the AI could categorise tissue into any of 13 common forms of brain tumours, such as malignant glioma, lymphoma, metastatic tumours, diffuse astrocytoma, and meningioma.
A clinical trial involving 278 brain tumour and epilepsy patients and three different medical institutions was then set up to test the efficacy of the system. SRH images were evaluated by either human experts or the AI. Looking at the results, the AI correctly identified the tumour 94.6 per cent of the time, while the human neuropathologists were accurate 93.9 per cent of the time. Interestingly, the errors made by humans were different than the errors made by the AI. This is actually good news, because it suggests the nature of the AI’s mistakes can be accounted for and corrected in the future, resulting in an even more accurate system, according to the authors.
“SRH will revolutionise the field of neuropathology by improving decision-making during surgery and providing expert-level assessment in the hospitals where trained neuropathologists are not available,” said Matija Snuderl, a co-author of the study and an associate professor at NYU Grossman School of Medicine, in the press release.
Also, because many of the histologic features seen in brain tumours are seen in other forms of cancer, this system could eventually be used in other fields and surgeries, including dermatology, gynecology, breast surgery, and head and neck surgery, according to the study.
[referenced url=” thumb=” title=” excerpt=”]
Slowly but surely, artificial intelligence is surpassing humans when it comes to this sort of thing. Google, for example, has systems that can diagnose both breast cancer and lung cancer better than human experts. We sometimes—and quite legitimately—get nervous about human-superior AI, but in cases such as these, bring ‘em on!