Here’s a feel-good story to carry you through the rest of the weekend. Veterinarians at Michigan State University say they were able to save the life of a one-year-old Rottweiler named Stella who had been horrifically burned, thanks in part to an innovative technology that uses fish skin to help the body heal itself.
Stella was trapped in a house fire this past February (her owners were away from home at the time). Though she survived, she was left with severe second- and three-degree burns over 10 per cent of her body, serious breathing problems caused by smoke inhalation, and scarred eyes. Upon arrival to the Michigan State University Veterinary Medical Center, her condition was critical.
Ordinarily, dogs like Stella would be put under general anaesthesia so that skin grafts can be easily placed onto the affected areas. But that wasn’t a realistic option for her, according to her doctors.
“We had to get creative with her burns because of the significant trauma to Stella’s lungs,” Brea Sandness, a veterinarian and surgical resident at MSU, said in a university release detailing Stella’s case. “She wasn’t a great candidate for anesthesia because of her respiratory injuries.”
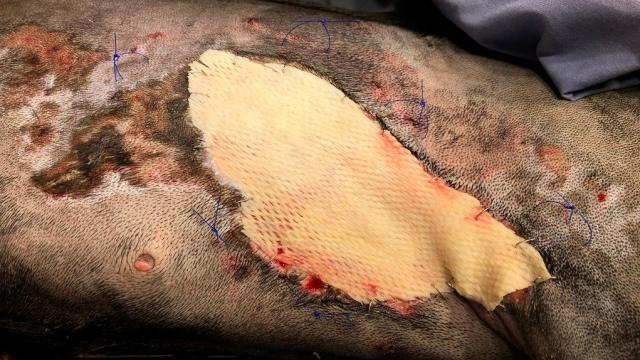
Instead, the MSU vets used fish skin grafts donated to them by the Virginia-based company Kerecis.
Fish skin has been explored as a skin substitute for people and animals in recent years. What makes it appealing is that, compared to skin grafts made from mammals, the risk of viral contamination is likely much lower. Several fish skin graft products, often made from tilapia, are currently being tested and deployed in hospitals, as well as during emergency crises such as the California wildfires last year.
But Kerecis claims its product — derived from the Icelandic cod fish — is even more efficient at regenerating skin due to how it’s processed. The fish skin is descaled, which is thought to make it more like living tissue, while it’s still filled with omega-3 fatty acids, which are known to reduce inflammation and promote wound healing.
With Stella, the fish skin was applied and replaced as needed with relative ease.
“We were able to place them on her with minimal sedation, which not only allowed us to heal her without additional stress to her lungs, but improved the way her burns healed,” said Sandness.
Stella ultimately spent two weeks at MSU, and another month healing up at home. Though she’s still on the mend and will likely need long-term care to manage her breathing and vision problems, she’s also healthy enough to move and walk around again.
The team credits the fish skin grafts for having helped her through the worst of it. So much so that they’ve decided to discuss her case at the Society of Veterinary Soft Tissue Surgery’s annual convention next month.
“Stella’s case is an inspiration, and her grafts have the potential to be a new and highly effective treatment tool in the veterinary profession,” Sandness said. “She’s a living example that the fire within her burned stronger than the fire that injured her.”
Earlier this April, Kerecis also announced preliminary positive trial results for its skin grafts being used on human patients as well.