Lots of elements factor into whether a community suffers higher rates of asthma. There’s even a genetic component.
When Anthony Nardone, a medical student in the University of California at San Francisco and Berkeley’s Joint Medical Program, first began learning about the mechanisms that lead to health disparities, he began to wonder about the role history plays, particularly the U.S. history of segregation.
On Wednesday, Nardone presented research at the annual American Thoracic Society Conference that shows how segregation may be, in part, to blame for higher rates of asthma emergency room visits for residents in some neighbourhoods in California. The research takes a deep dive into redlining, a particularly problematic part of urban history still with us today.
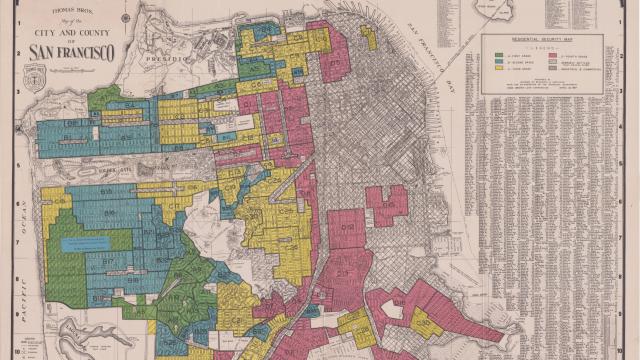
Redlining is a practice where the Federal Housing Authority literally drew red lines around black and brown communities and labelled them as “risky” investments that was prevalent from the 1930s through the 1970s.
This not only made it hard for people in these neighbourhoods to be approved for home loans and, in turn, build wealth. It also encouraged businesses to disinvest in those communities. It’s why a lot of white homeowners today still live where there aren’t many (if any) people of colour, and why you’ll struggle to find a cute smoothie shop or boutique in a poor black community.
Nardone wanted to see what other legacies this discriminatory practice left, especially on people’s health. His research uncovered that eight California cities—including San Francisco, Oakland, and Los Angeles—with a history of redlining are twice as likely as their white neighbours to visit emergency rooms for asthma.
He and his team conducted the study using historic redlining maps available on the University of Richmond’s “Mapping Inequality” project and comparing them to individual census tracts. They categorized tracts as redlined or not.
Then, Nardone and his team were able to look at the number of emergency room visits for asthma and air quality data by census tract, which they gathered from state records.
The results show asthma-related emergency room visits were higher in historically redlined communities. They also saw nearly twice the level of diesel particulate matter in the air compared to neighbourhoods that were categorized as “low risk” under these racist policies.
“This suggests that there are complex long-term consequences of redlining shaping neighbourhoods,” Nardone told Earther.
It’s hard to tell exactly why the number of asthma-related hospital visits are higher, but Nardone believes history plays a key role. Redlining contributes to why many black and brown families still struggle to build wealth, which can prevent them from buying better quality homes that have less indoor air pollution. All of these are factors that can contribute to a person’s health.
The researchers still need to do further analyses to solidify their case. They plan to look at individual health data next to see if this pattern is seen across individuals in these communities and compare it to individuals from non-redlined communities.
There’s also the chance that ongoing gentrification in these cities skewed their results. Nardone thinks the number of emergency room visits could have been higher before the influx of white people into many of these communities.
He hopes to take his research outside of California and see if this pattern exists in other states. If it does, it would be the latest evidence in a long-standing saga of environmental racism.