In 2017, a team of Australian and Japanese scientists announced a breakthrough that could someday save the lives of countless babies.
They used an artificial womb to keep premature lamb fetuses alive and healthy enough for them to be later delivered without serious health complications. This month, that same team announced a leap forward in their technology, now claiming it can keep even extremely premature lambs alive.
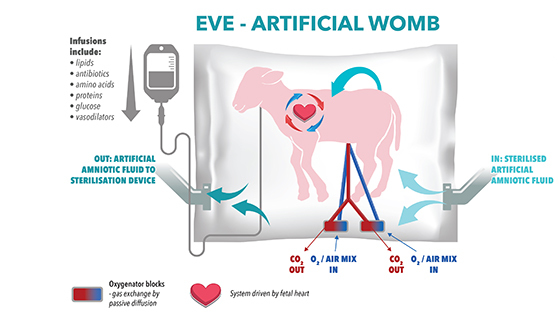
Their artificial womb is called the ex-vivo uterine environment (EVE) therapy. On its surface, it looks like a pillowcase-sized, transparent bag. Once the foetus is inside EVE, though, it is surrounded by a protective bath of sterilized, artificial amniotic fluid, which is routinely filtered out and replaced.
Infusions of vital nutrients like amino acids and medications like antibiotics are regularly provided via IV. The womb also acts as a lung, pumping out carbon dioxide and pumping in fresh air.
Lambs are a popular model for studying prenatal humans because their development in the womb is similar to ours but sped along. Compared to the nine-month gestation period for humans, healthy newborn lambs are typically delivered in 150 days, or slightly less than five months.
So far, studies of artificial wombs, including the team’s earlier experiments with EVE, have used lambs at around 107 to 115 days of development. That time period roughly equates to late-term premature human babies. But while these children definitely need special care once delivered, modern medicine is already good at keeping them alive, with survival rates ranging around 90 per cent.
We’re much less capable of keeping alive babies born between 22 to 24 weeks of development, a period considered the border of viability. And it’s these children who would benefit most from an artificial womb that can bridge the crucial gap to normal development if it ever became reality.
The team behind this new study, published this month in The American Journal of Obstetrics & Gynecology (AJOG), say theirs is the first documented attempt to successfully reach this extra step with lambs.
Eight lamb fetuses at 95 days of development were placed inside EVE for 120 hours, or roughly five days. Their health was compared to a control group of lamb fetuses at 100 days of development. Ultimately, seven of the extremely premature lamb fetuses survived the entire five days of EVE therapy.
These survivors were just as healthy and developed as the control group was, indicating that EVE was able to mimic the conditions of the womb well enough even for these especially fragile fetuses. In order to compare them, both groups were euthanised at 100 days.
“In the AJOG study, we have proven the use of this technology to support, for the first time, extremely preterm lambs equivalent to 24 weeks of human gestation in a stable, growth-normal state for five days,” senior study author Matthew Kemp, an associate professor of obstetrics and gynecology at the University of Western Australia and head of the Perinatal Research Laboratories at the Women and Infants Research Foundation, said in a statement.
“This result underscores the potential clinical application of this technology for extremely preterm infants born at the border of viability. In the world of artificial placenta technology, we have effectively broken the 4 minute mile.”
Kemp’s team isn’t the only one that has made great strides recently in refining the artificial womb, a concept that’s existed theoretically for decades. Researchers at Children’s Hospital of Philadelphia published research on their own artificial womb, the Biobag, in 2017.
They claimed their technology could support lamb fetuses for as long as 28 days, and successfully led to normally developed lambs that, as of 2017, were still alive and thriving.
At this time, though, we’re likely still years off from any human trials. And aside from technological hurdles, researchers will need to fend off criticism that their technology is ultimately intended to replace natural births or could have other unintended consequences, like limiting abortion rights.
“There is no technology, even on the horizon, that can support the foetus from the embryonic stage,” Alan Flake from the Children’s Hospital of Philadelphia, said at the time of their study’s release in 2017.