In recent years, superbugs have become one of the biggest threats to modern human health. At present, the CDC estimates that some 23,000 people die every year from multidrug-resistant infections in the United States. The threat of antibiotic-resistant bacteria to global health is big enough that this year the World Health Organisation for the first time published a list of the 12 superbugs that pose the greatest threat to humans.
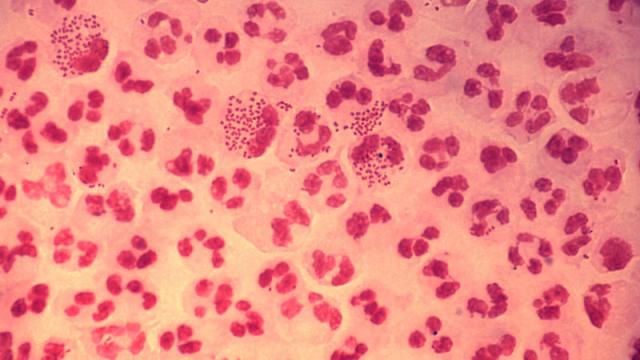
Gonococcal urethritis under the microscope. Image: Wikimedia
Now new research from Sweden sheds some light onto how bacteria evolve resistance to antibiotics: genetics.
Researchers from Chalmers University of Technology and the University of Gothenburg in Sweden combed through large volumes of bacterial DNA and uncovered 76 previously unknown genes that help make bacteria resistant to last-resort antibiotics. The results of their work were published this month in the journal Microbiome.
Several of the genes uncovered in the new work provide bacteria with the ability to fight carbapenems, the most powerful class of antibiotics used to treat bacteria that has already grown resistant to multiple antibiotics.
Information about how bacteria develops antibiotic resistance, they hope, will lead to the development of new drugs that will be more effective. Perhaps, for example, a drug could be developed to turn off that gene that allows bacteria to resist antibiotics in the first place.
The genes they discovered, they wrote, are just the beginning. Next, they will search for genes that also enable resistance to other forms of antibiotics.
Their research cannot come soon enough. Already three families of bacteria — Acinetobacter, Pseudomonas and various Enterobacteriaceae — that often appear in hospitals and nursing homes have evolved resistance to carbapenems. After carbapenems fail to treat an infection, there is typically little else that doctors can do.