Reviving unresponsive patients has long been a dream of humanity, and an oft-talked about part of the human condition. Maybe you’ve cried along with the movie Awakenings, or had long conversations with relatives about what happens should you or they end up in the same position.
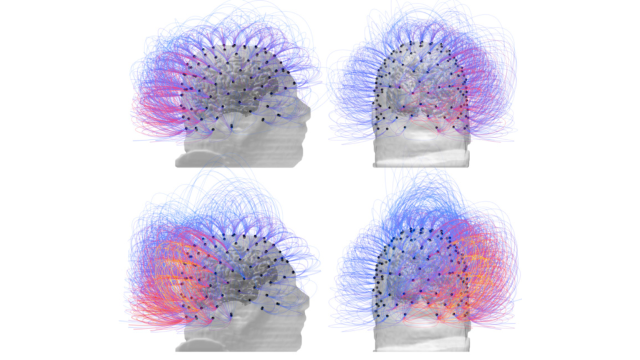
Information sharing between brain cells before (top) and after (bottom) Image: Corazzol et al (2017)
But these conversations would be much different if you could restore consciousness, as a new paper claims to do… kind of. A French patient received a traumatic brain injury 15 years ago, putting him into a vegetative state. After stimulating a part of the brain, scientists were seemingly able to restore some of the patients’ consciousness. But no, we’re not quite at Awakenings yet.
A vegetative state is not a coma. Instead, the brain-damaged patient is awake but unaware and conscious-less. A paper in BMC Medicine describes the condition as “only showing reflex movements without response to command”. Put very simply, researchers are pretty sure the condition has something to do with brain damage altering how electrical signals travel between the inner and outer sections of the brain, as well as around the outer layer. Some patients recover from vegetative states, but others don’t.
The scientists hypothesised that perhaps stimulating the vagus nerve, the longest nerve connected directly to the brain, would help rewire parts of the brain and allow for higher levels of consciousness. They implanted a stimulator to the nerve and applied a current, slowly ramping it up over a month. Afterwards, they noticed the patient had increased brain activity and observed him move from the vegetative to a minimally conscious state — as one paper describes, “a condition of severely altered consciousness in which minimal but definite behavioural evidence of self or environmental awareness is demonstrated.”
The patient’s behaviour on the “Coma Recovery Scale” went from five to 10 (the maximum score is a 23), with the greatest increases in how his eyes reacted to stimuli. New Scientist reports that the patient showed an emotional response to music, moved his cheek in response to instructions to smile, and opened his eyes wide in response to the researchers moving in close.
This is obviously promising. As the authors conclude in the work published in Current Biology, “our study demonstrates the therapeutic potential of vagus nerve stimulation to modulate large-scale human brain activity and alleviate disorders of consciousness.”
James L. Bernat, a professor of neurology and medicine at Dartmouth, told CNN that the study was provocative, but especially praised the choice of patient. Using a patient in a vegetative state for 15 years versus someone only in the state for a few months decreases the chance that the authors would have observed the patient improving on his own. Bernat points out that every vegetative state case is different, and the vagus nerve stimulation might not work for every patient.
Other researchers agreed with that sentiment. “Vagal nerve stimulation may not be a general treatment. Its effectiveness depends on the nature of brain lesion,” György Buzsaki, a neuroscience professor at New York University told Gizmodo in an email. “On the positive side, these are welcome findings because vagus nerve stimulation is a relatively simple method. In principle, the nerve can be stimulated percutaneously as well. Therefore, it can be tested in other patients as well without brain surgery.”
But Buzsaki thought that important details were missing from the new paper — and again reminded me that the patient is minimally conscious scientifically, not awake or conscious by a regular person’s definition of the word. “Stimulation resulted in ‘general arousal, sustained attention, body motility and visual pursuit’ and scores on the Coma Recovery Scale-Revised ‘as reported by clinicians and family members’,” he said. “This does not mean that the person could say “I am Joe” or ask the question “Where am I?” verbally or by other means.
This is definitely a promising case study with tantalising results — but it’s just a one-time thing. As always with a single case study, it might not as incredible as some headlines imply.
“Investigators… should be more cautious not to imply false expectation in family members that further improvement beyond visual pursuit and occasional facial response is guaranteed,” said Buzsaki. “Despite these caveats, this is important progress in the right direction.”