Egg freezing has recently jumped from an expensive and rare medical procedure to a recognised backup plan for women pushing up against the biological cutoff for conception. But what exactly are you signing up for?
As a career perk, putting baby-making cells on ice is stirring up controversy (and plenty of 30-year-old women would not be happy to receive an egg freezing credit wrapped up in a bow). A fertility doctor recently went so far as proclaiming oocyte preservation as the “perfect 30th birthday gift” for women and Facebook, NASA and Apple are now offering to cover egg freezing as part of female employees’ insurance.
As a medical process, however, it’s a remarkable, futuristic way to reschedule the deadlines set by our bodies.
The path to motherhood is paved with hormone needles
For a woman to conceive with frozen eggs, first she needs to make a bunch of extra ones. This means taking a round of follicle-stimulating hormones to accelerate how many eggs her body gets ready.
After the hormone/PMS-symptom/needle/nightmare saga, doctors generally extract the eggs around 36 hours after the final injection. They knock you out and use a needle attached to the ultrasound probe that makes the hormone needles look like little sharp toys to reach the follicles within the ovaries. The process collects the fluid within the follicle. The eggs are in the fluid.
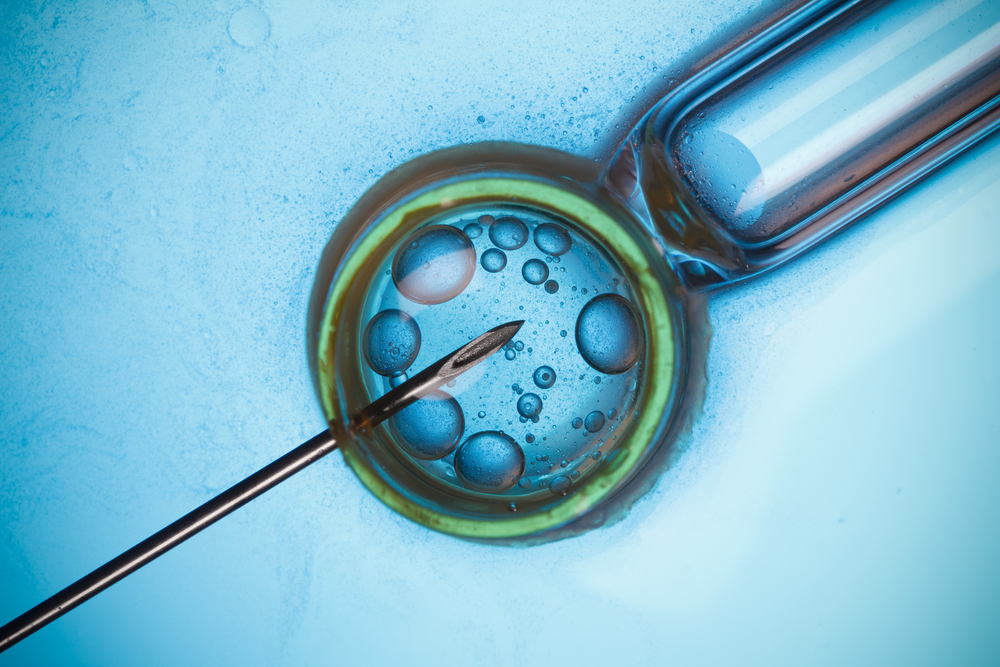
In-vitro concept art. Image: Sukharevskyy Dmytro (nevodka) via Shutterstock
After that, there’s not much more for the woman to do but wait for the right time to procreate (and shell out for regular maintenance fees to preserve the eggs). The doctors, however, are far from finished. They need to isolate and freeze the eggs within a short window of time, before they’re no longer viable.
A long day’s journey into the liquid nitrogen

This window is very narrow. But while the process for producing the eggs has been largely the same since in-vitro fertilization started years ago, the process for keeping them cold has dramatically improved in recent years.
Doctors originally had trouble freezing eggs without harming them because the water inside the eggs would form ice crystals as they froze.
“An egg is made mostly of water, so it’s the largest cell in the body, and when you freeze an egg, the goal is to dehydrate it, to take all the water out of it so that it shrinks, and then we put it in liquid nitrogen,” Dr Jane Frederick, a fertility doctor in Newport, California, told me.
“The worst thing that can happen is the formation of something called ice crystals,” she continued. “You can imagine a balloon filled with water. The ice crystals are like sharp pinpricks that can damage the membrane, so when you try to rehydrate the egg, when you want to thaw it, the membranes will get damage and the cell will no longer be viable.”
Over the past 8 to 10 years a process cropped up that offered a better solution to the jabbing ice crystal dilemma. It’s called vitrification, and it’s much faster than the slow-freezing process. Instead, doctors transfer the eggs into a container where they are cooled quickly by liquid nitrogen, so quickly that there’s no time for the crystals to form. “So now we’re seeing about 80 per cent survival on the eggs that are being thawed,” Frederick said.

Oocyte and embryo vitrification. Image: Pacific Fertility Center
The cryoprotectant is a type of antifreeze, so the doctors basically give eggs a bath in a solution that’s kind of like whatever it is Jabba the Hutt dunks Han Solo in in The Empire Strikes Back. They’re instantly frozen, there are no killer ice crystals, and like Han, it’s possible to revive them at a later date.
Since the antifreeze cools at such a rapid speed — up to 70,000 times faster than the slow-freezing process — the bath phase often has two parts, with the eggs first being placed in a solution with a lower concentration of antifreeze and then in the higher concentration.
Fertility clinics and hospitals typically store the eggs on-site. To keep them cold, they’re encased in liquid nitrogen, which is cooled to around -196°C which is so cold I just shivered thinking about it.
The liquid nitrogen tanks are attended daily by staff, which is one of the reasons maintaining the freezing service costs money each year. The egg trays look like straws, and each facility has slightly different ways of arranging them, but keeping them at the -196°C is crucial.

To freeze or not to freeze
As people like Dr Frederick continue to streamline and improve the egg freezing process, the likelihood of safely extending the age you can begin motherhood goes up.
USC estimates that around 2000 babies have been born from frozen eggs, and while the studies that have been conducted show no evidence that there’s an increased risk of birth defects, the relative newness of the procedure means there’s so much we don’t know. If giving birth from a frozen egg goes mainstream, doctors will have more opportunities to improve the process further.
Doctors in Italy pioneered vitrification for eggs because embryo freezing is not allowed there, so egg freezing is more common than other parts of the world. The method represents a huge jump from the slow freezing, and it shows the kind of medical leaps that can happen when doctors prioritise the procedure. Technological advancement in fertility preservation is inevitably linked to a cultural acceptance of the option as a logical alternative to getting pregnant at a younger age. However until that happens, egg freezing remains complicated, risky, and expensive.
A round of egg freezing costs around $US10,000, plus there are annual maintenance fees to keep the eggs frozen. Keep those puppies on ice for a decade and you’re looking at upwards of $US20,000 for the whole process, if not a lot more. That’s a big chunk (or all!) of your future kid’s college education right there. And if you need to do a second round, well, your bank account may start bleeding from the eyes.
There’s no set “right number” of eggs to freeze; most women go for between 12 to 30. Each time eggs are collected, doctors average somewhere between 8-14 eggs, so people who want to stockpile will need more than one round.

Vitrification products for oocytes, zygotes, embryos. Image: Kitazato/Dibimed
If employers do start subsidizing the process, egg storage as a backup plan could become as common as popping a daily dose of hormonal birth control. Fertility doctors have been reporting an uptick in women wanting more information on freezing their eggs for non-medical reasons in the past year. After all, if money isn’t the issue, why not? It’s a safety net for any woman worried her body’s fertility peaks won’t coincide with any of the other stuff you want when you’re going to have a child, like savings or a life partner.
On the other hand, the process is not foolproof. Freezing eggs out of necessity — like before surgery or a harsh round of chemotherapy — can preserve a person’s ability to have biological children. But neither the American College of Obstetricians and Gynecologists nor the American Society for Reproductive Medicine approve of egg freezing as a way to defer childbearing. The ASRM did take the ‘experimental’ label off egg freezing, but only for women doing it for medical reasons, and it found a “lack of data on safety, efficacy, cost-effectiveness, and potential emotional risks.”
None of us have control over our bodies. We try to stave off their decline with jogs and smoothies and optimism. Most of them get fatter and flabbier than we’d like. They emit embarrassing noises and smells, they age, they get soft and brittle at the same time.
For women, controlling the body’s reproductive path can change and save lives. Contraceptives have done just that, and now egg freezing is becoming something that average women are starting to consider. The medical risks of jacking yourself up with hormones remain high enough to act as an understandable deterrent. But in the right circumstances, a successful, affordable process can feel like a miracle, a sort of stopwatch for the biological clock. A way to trick time.
Photos on the left courtesy of HRC Fertility Clinic/ Header art by Jim Cooke
