In the war against malaria, one small corner of the globe has repeatedly turned the tide, rendering our best weapons moot and medicine on the brink of defeat. Ed Yong reports.
The meandering Moei river marks the natural boundary between Thailand and Myanmar. Its muddy waters are at their fullest, but François Nosten still crosses them in just a minute, aboard a narrow, wooden boat. In the dry season, he could wade across. As he steps onto the western riverbank, in Myanmar, he passes no checkpoint and presents no passport.
The air is cool. After months of rain, the surrounding jungle pops with vivid lime and emerald hues. Nosten climbs a set of wooden slats that wind away from the bank, up a muddy slope. His pace, as ever, seems relaxed and out of kilter with his almost permanently grave expression and urgent purpose. Nosten, a rangy Frenchman with tousled brown hair and glasses, is one of the world’s leading experts on malaria. He is here to avert a looming disaster. At the top of the slope, he reaches a small village of simple wooden buildings with tin and thatch roofs. This is Hka Naw Tah, home to around 400 people and a testing ground for Nosten’s bold plan to completely stamp out malaria from this critical corner of the world.
Malaria is the work of the single-celled Plasmodium parasites, and Plasmodium falciparum chief among them. They spread between people through the bites of mosquitoes, invading first the liver, then the red blood cells. The first symptoms are generic and flu-like: fever, headache, sweats and chills, vomiting. At that point, the immune system usually curtails the infection. But if the parasites spread to the kidneys, lungs and brain, things go downhill quickly. Organs start failing. Infected red blood cells clog the brain’s blood vessels, depriving it of oxygen and leading to seizures, unconsciousness and death.
When Nosten first arrived in South-east Asia almost 30 years ago, malaria was the biggest killer in the region. Artemisinin changed everything. Spectacularly fast and effective, the drug arrived on the scene in 1994, when options for treating malaria were running out. Since then, “cases have just gone down, down, down,” says Nosten. “I’ve never seen so few in the rainy season — a few hundred this year compared to tens of thousands before.”

But he has no time for celebration. Artemisinin used to clear P. falciparum in a day; now, it can take several. The parasite has started to become resistant. The wonder drug is failing. It is the latest reprise of a decades-long theme: we attack malaria with a new drug, it mounts an evolutionary riposte.
Back in his office, Nosten pulls up a map showing the current whereabouts of the resistant parasites. Three coloured bands highlight the borders between Cambodia and Vietnam, Cambodia and Thailand, and Thailand and Myanmar (Burma). Borders. Bold lines on maps, but invisible in reality. A river that can be crossed in a rickety boat is no barrier to a parasite that rides in the salivary glands of mosquitoes or the red blood cells of humans.
History tells us what happens next. Over the last century, almost every frontline antimalarial drug — chloroquine, sulfadoxine, pyrimethamine — has become obsolete because of defiant parasites that emerged from western Cambodia. From this cradle of resistance, the parasites gradually spread west to Africa, causing the deaths of millions. Malaria already kills around 660,000 people every year, and most of them are African kids. If artemisinin resistance reached that continent, it would be catastrophic, especially since there are no good replacement drugs on the immediate horizon.
Nosten thinks that without radical measures, resistance will spread to India and Bangladesh. Once that happens, it will be too late. Those countries are too big, too populous, too uneven in their health services to even dream about containing the resistant parasites. Once there, they will inevitably spread further. He thinks it will happen in three years, maybe four. “Look at the speed of change on this border. It’s exponential. It’s not going to take 10 or 15 years to reach Bangladesh. It will take just a few. We have to do something before it’s too late.”
Hundreds of scientists are developing innovative new ways of dealing with malaria, from potential vaccines to new drugs, genetically modified mosquitoes to lethal fungi. As Nosten sees it, none of these will be ready in time. The only way of stopping artemisinin resistance, he says, is to completely remove malaria from its cradle of resistance. “If you want to eliminate artemisinin resistance, you have to eliminate malaria,” says Nosten. Not control it, not contain it. Eliminate it.
That makes the Moei river more than a border between nations. It’s Stalingrad. It’s Thermopylae. It’s the last chance for halting the creeping obsolescence of our best remaining drug. What happens here will decide the fate of millions.
The world tried to eliminate malaria 60 years ago. Malaria was a global affliction back then, infecting hundreds of thousands of troops during World War II. This helped motivate a swell of postwar research. To fight the disease, in 1946 the USA created what is now the Centres for Disease Control and Prevention (CDC), the country’s premier public health institute. After a decisive national eradication programme, the nation became malaria-free in 1951. Brazil had also controlled a burgeoning malaria epidemic with insecticides.

Meanwhile, new weapons had emerged. The long-lasting insecticide DDT was already being widely used and killed mosquitoes easily. A new drug called chloroquine did the same to Plasmodium. Armed with these tools and buoyed by earlier successes, the World Health Organisation formally launched the Global Malaria Eradication Programme in 1955. DDT was sprayed in countless homes. Chloroquine was even added to table salt in some countries. It was as ambitious a public health initiative as has ever been attempted.
It worked to a point. Malaria fell dramatically in Taiwan, Sri Lanka, India, the Caribbean, the Balkans, and parts of the south Pacific. But ultimately the problem was too big, the plan too ambitious. It barely made a dent in sub-Saharan Africa, where public health infrastructure was poor and malaria was most prevalent. And its twin pillars soon crumbled as P. falciparum evolved resistance to chloroquine and mosquitoes evolved resistance to DDT. The disease bounced back across much of Asia and the western Pacific.
In 1969, the eradication programme was finally abandoned. Despite several successes, its overall failure had a chilling impact on malaria research. Investments from richer (and now unaffected) countries dwindled, save for a spike of interest during the Vietnam War. The best minds in the field left for fresher challenges. Malaria, now a tropical disease of poor people, became unfashionable.
François Nosten always wanted to travel. His father, a sailor on merchant ships, returned home with stories of far-flung adventures and instilled a deep wanderlust. Nosten’s original plan was to work on overseas development projects, but one of his teachers pushed him down a different path. “He said the best thing you can do if you want to travel anywhere is to be a doctor. That’s why I started medical school.” As soon as he graduated, he joined Médecins Sans Frontières and started living the dream. He flew off to Africa and South-east Asia, before arriving in Thailand in 1983. There, he started treating refugees from Myanmar in camps along the Thai border.
In 1985, an English visitor arrived at the camps and Nosten took him for a random tourist until he started asking insightful questions about malaria. That man was Nick White. A British clinician, he was drawn to Bangkok in 1980 by the allure of the tropics and a perverse desire to study something unfashionable. The University of Oxford had just set up a new tropical medicine research unit in collaboration with Bangkok’s Mahidol University, and White was the third to join.
“The rosbif and the frog”, as Nosten puts it, bonded over an interest in malaria, a desire to knuckle down and get things done, and a similar grouchy conviviality. They formed a close friendship and started working together.
In 1986, they set up a field station for White’s Bangkok research unit: little more than a centrifuge and microscope within Nosten’s rickety house. Three years later, Nosten moved to Shoklo, the largest refugee camp along the Thai — Myanmar border and home to around 9,000 people. Most were Karen — the third largest of Myanmar’s 130 or so ethnic groups — who were fleeing persecution from the majority Bamar government. Nosten worked out of a bamboo hospital — the first Shoklo Malaria Research Unit.
Malaria was rife. Floods were regular. Military leaders from both Thailand and Myanmar occasionally ordered Nosten to leave. Without any electricity, he often had to use a mirror to angle sunlight into his microscope. He loved it. “I’m not a city person,” he says. “I couldn’t survive in Bangkok very well. I wasn’t alone in Shoklo but it was sufficiently remote.” The immediacy of the job and the lack of bureaucracy also appealed. He could try out new treatments and see their impact right away. He trained local people to detect Plasmodium under a microscope and help with research. He even met his future wife — a Karen teacher named Colley Paw, who is now one of his right-hand researchers (White was the best man at their wedding). These were the best years of his life.
The Shoklo years ended in 1995 after a splinter faction of Karen started regularly attacking the camps, in a bid to force the refugees back into Myanmar. “They came in and started shooting,” says Nosten. “We once had to hide in a hole for the night, with bullets flying around.” The Thai military, unable to defend the scattered camps, consolidated them into a single site called Mae La — a dense lattice of thatch-roofed houses built on stilts, which now contains almost 50,000 people. Nosten went with them.

He has since expanded the Shoklo Unit into a huge hand that stretches across the region. Its palm is a central laboratory in the town of Mae Sot, where Nosten lives, and the fingers are clinics situated in border settlements, each with trained personnel and sophisticated facilities. The one in Mae La has a $US250,000 neonatal care machine, and can cope with everything short of major surgery. Nosten has also set up small ‘malaria posts’ along the border. These are typically just volunteer farmers with a box of diagnostic tests and medicine in their house.
“I don’t know anybody else who could have done what François has done,” says White. “He’ll underplay the difficulties but between the physical dangers, politics, logistical nightmares, and the fraught conditions of the refugees, it’s not been easy. He’s not a shrinking violet.”
Thanks to Nosten’s network, locals know where to go if they feel unwell, and they are never far from treatments. That is vital. If infected people are treated within 48 hours of their first symptoms, their parasites die before they get a chance to enter another mosquito and the cycle of malaria breaks. “You deploy early identification and treatment, and malaria goes away,” says Nosten. “Everywhere we’ve done this, it’s worked.”
Victories in malaria are often short-lived. When Nosten and White teamed up in the 1980s, their first success was showing that a new drug called mefloquine was excellent at curing malaria, and at preventing it in pregnant women. Most drugs had fallen to resistant parasites and the last effective one — quinine — involved a week of nasty side-effects. Mefloquine was a godsend.
But within five years, P. falciparum had started to resist it too. “We tried different things like increasing the dose, but we were clearly losing the drug,” says Nosten. “We saw more and more treatment failures, patients coming back weeks later with the same malaria. We were really worried that we wouldn’t have any more options.”
Salvation came from China. In 1967, Chairman Mao Zedong launched a covert military initiative to discover new antimalarial drugs, partly to help his North Vietnamese allies, who were losing troops to the disease. It was called Project 523. A team of some 600 scientists scoured 200 herbs used in traditional Chinese medicine for possible antimalarial chemicals. They found a clear winner in 1971 — a common herb called qing hao (Artemisia annua or sweet wormwood). Using hints from a 2,000-year-old recipe for treating haemorrhoids, they isolated the herb’s active ingredient, characterised it, tested it in humans and animals, and created synthetic versions. “This was in the aftermath of the Cultural Revolution,” says White. “Society had been ripped apart, there was still a lot of oppression, and facilities were poor. But they did some extremely good chemistry.”
The results were miraculous. The new drug annihilated even severe forms of chloroquine-resistant malaria, and did so with unparalleled speed and no side-effects. The team named it Qinghaosu. The West would know it as artemisinin. Or, at least, they would when they found out about it.
Project 523 was shrouded in secrecy, and few results were published. Qinghaosu was already being widely used in China and Vietnam when the first English description appeared in the Chinese Medical Journal in 1979. Western scientists, suspicious about Chinese journals and traditional medicine, greeted it with scepticism and wasted time trying to develop their own less effective versions. The Chinese, meanwhile, were reluctant to share their new drug with Cold War enemies.
During this political stalemate, White saw a tattered copy of the 1979 paper. He travelled to China in 1981, and returned with a vial of the drug, which he still keeps in a drawer in his office. He and Nosten began studying it, working out the right doses, and testing the various derivatives.
They realised that artemisinin’s only shortcoming was a lack of stamina. People clear it so quickly from their bodies that they need seven daily doses to completely cure themselves. Few complete the full course. White’s ingenious solution was to pair the new drug with mefloquine — a slower-acting but longer-lasting partner. Artemisinin would land a brutal shock-and-awe strike that destroyed the majority of parasites, mefloquine would mop up the survivors. If any parasites resisted the artemisinin assault, mefloquine would finish them off. Plasmodium would need to resist both drugs to survive the double whammy, and White deemed that unlikely. Just three days of this artemisinin combination therapy (ACT) was enough to treat virtually every case of malaria. In theory, ACTs should have been resistance-proof.
Nosten started using them along the Thai — Myanmar border in 1994 and immediately saw results. Quinine took days to clear the parasites and left people bed-ridden for a week with dizzy spells. ACTs had them returning to work after 24 hours.
But victories in malaria are often short-lived. In the early 2000s, the team started hearing rumours from western Cambodia that ACTs were becoming less effective. White tried to stay calm. He had heard plenty of false alarms about incurable Cambodian patients, but it always turned out that they were taking counterfeit drugs. “I was just hoping it was another of those,” he says.
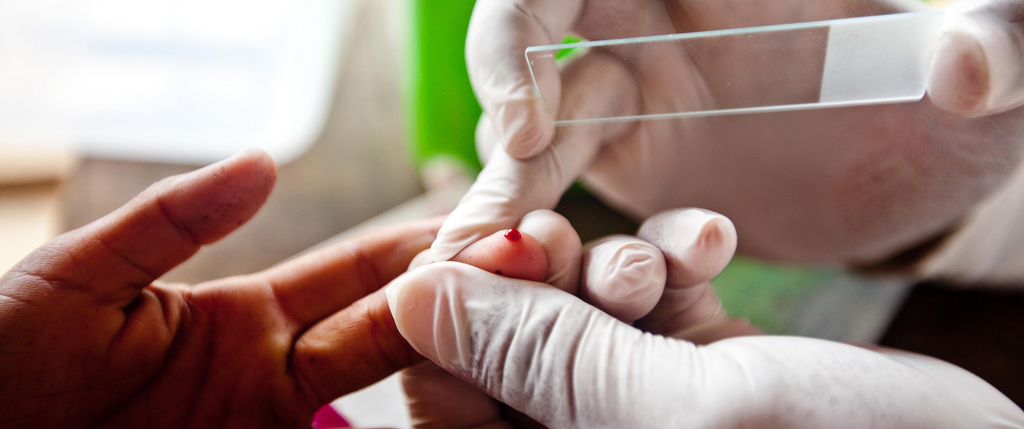
It was not. In 2006, Harald Noedl from the Medical University of Vienna started checking out the rumours for himself. In the Cambodian village of Ta Sanh, he treated 60 malaria patients with artesunate (an artemisinin derivative) and found that two of them carried exceptionally stubborn parasites. These infections cleared in four to six days, rather than the usual two. And even though the patients stayed in a clinic outside any malaria hotspots, their parasites returned a few weeks later.
“I first presented those data in November 2007 and as expected, people were very sceptical,” says Noedl. After all, a pair of patients is an epidemiological blip. Still, this was worrying enough to prompt White’s team to run their own study in another nearby village. They got even worse news. The 40 people they treated with artesunate took an average of 3.5 days to clear their parasites, and six of them suffered from rebounding infections within a month. “Rapid parasite clearance is the hallmark of artemisinins,” says Arjen Dondorp, one of White’s colleagues based in Bangkok. “That property suddenly disappeared.”
Despite the hopes that ACTs would forestall artemisinin’s expiry, resistance had arrived, just as it had done for other antimalarials. And, as if to rub salt in the wound, it had come from the same damn place.
Why has a small corner of western Cambodia, no bigger than Wales or New Jersey, repeatedly given rise to drug-beating parasites?
White thinks that the most likely explanation is the region’s unregulated use of antimalarial drugs. China supplied artemisinin to the tyrannical Khmer Rouge in the late 1970s, giving Cambodians access to it almost two decades before White conceived of ACTs. Few used it correctly. Some got ineffective doses from counterfeit pills. Others took a couple of tablets and stopped once their fever disappeared. P. falciparum was regularly exposed to artemisinin without being completely wiped out, and the most resistant parasites survived to spread to new hosts. There is a saying among malariologists: “The last man standing is the most resistant.”
Genetic studies hint at other explanations. Early last year, Dominic Kwiatkowski from the University of Oxford showed that some P. falciparum strains from west Cambodia have mutations in genes that repair faults in their DNA, much like some cancer cells or antibiotic-resistant bacteria. In other words, they have mutations that make them prone to mutating. This might also explain why, in lab experiments, they develop drug resistance more quickly than strains from other parts of the world. Evolution is malaria’s greatest weapon, and these ‘hypermutators’ evolve in fifth gear.
Kwiatkowski’s team also found that P. falciparum is spookily diverse in west Cambodia. It is home to three artemisinin-resistant populations that are genetically distinct, despite living in the same small area. That is bizarre. Without obvious barriers between them, the strains ought to regularly mate and share their genes. Instead, they seem to shun each other’s company. They are so inbred that they consist almost entirely of clones.
Kwiatkowski suspects that these parasites descended from some lucky genetic lottery winners that accumulated the right sets of mutations for evading artemisinin. When they mate with other strains, their winning tickets break up and their offspring are wiped out by the drug. Only their inbred progeny, which keep the right combinations, survive and spread.
It undoubtedly helps that South-east Asia does not have much malaria. In West Africa, where transmission is high, a child might be infected with three to five P. falciparumstrains at any time, giving them many opportunities to mate and shuffle their genes. A Cambodian child, however, usually sees one strain at a time, and is a poor hook-up spot for P. falciparum. The region’s infrastructure may also have helped to enforce the parasites’ isolation: local roads are poor, and people’s movements were long constrained by the Khmer Rouge.
West Cambodia, then, could be rife with P. falciparum strains that are especially prone to evolving resistance, that get many opportunities to do so because antimalarial drugs are abused, and that easily hold on to their drug-beating mutations once they get them.
These are plausible ideas, but hard to verify since we still know very little about how exactly the parasites resist a drug. Earlier cases of resistance were largely due to mutations in single genes — trump cards that immediately made for invincible parasites. A small tweak in the crt gene, and P. falciparum can suddenly pump chloroquine out of its cells. A few tweaks to dhps and dhfr, the genes targeted by sulfadoxine and pyrimethamine, and the drug can no longer stick to its targets.
Artemisinin seems to be a trickier enemy. Curiously, P. falciparum takes a long time to evolve resistance to artemisinin in lab experiments, much longer than in the wild. Those strains that do tend to be weak and unstable. “I suspect you need a complicated series of genetic changes to make a parasite that’s not lethally unfit in the presence of these drugs,” says White. “It would be unusual if this was a single mutation.”
Practices such as unregulated drug use and misuse may help encourage and accelerate the rate of such changes out in the field. Kwiatkowski’s study suggests that the parasites may have evolved artemisinin resistance several times over, perhaps through a different route each time. Several groups are racing to find the responsible mutations, with news of the first few breaking in December 2013. That’s the key to quickly identifying resistant parasites and treating patients more efficiently. (Currently, you can only tell if someone has artemisinin-resistant malaria by treating them and seeing how long they take to get better.) “We want to be able to track resistance using blood spots on filter paper,” says Chris Plowe at the University of Maryland School of Medicine, whose group is one of those in the race.

But time is running out. From its origins in Cambodia, resistance has reached the Thai — Myanmar border. Nosten has shown that the proportion of patients who are still infected after three days of ACT has increased from zero in 2000 to 28 per cent in 2011. Most are still being cured, but as artemisinin becomes less effective, its partner drug will have to mop up more surviving parasites. Plasmodium will evolve resistance to the partner more quickly, driving both drugs towards uselessness.
This is already happening in western Cambodia, where ACTs are failing up to a quarter of the time and many people are still infected a month later. Long-lasting infections will provide parasites with more chances to jump into mosquitoes, and then into healthy humans. Malaria cases will rise. Deaths will follow. “This is the silence before the storm,” says Arjen Dondorp. “The threat is still slightly abstract and there’s still not that much malaria, which doesn’t help with a sense of urgency. If we suddenly see malaria exploding, then it will be a clear emergency, but it will also be too late.”
In his office at Mahidol University, Nick White is surrounded by yellowing monographs of old malaria research and overlooked by a wall-mounted mosaic of drug packets made by his daughter. He is now the chairman of the Mahidol — Oxford Tropical Medicine Research Unit and a mentor to the dozens of researchers within. He is gently ranting.
“Everything to do with change in malaria meets with huge resistance,” he says. He means political resistance, not the drug kind. He means the decade it took for the international community to endorse ACTs despite the evidence that they worked. He means the “treacle of bureaucracy” that he and Nosten swim through in their push to eliminate malaria.
“The global response to artemisinin resistance has been a bit pathetic. Everyone will tell you how important it is and there have been any number of bloody meetings. But there is little appetite for radical change.” He misses the old days when “you could drive a Land Rover across borders in your khaki shorts and spray things and do stuff”.
From the outside, things look rosier. Malaria is fashionable again, and international funding has gone up by 15 times in the last decade. Big organisations seem to be rallying behind the banner of elimination. In April 2013, the World Health Organisation published a strategy called The Emergency Response to Artemisinin Resistance…
“It’s a marvellous plan,” he says drily. “It says all the right things, but we haven’t done anything.” It follows two other strategies that were published in 2011 and 2012, neither of which slowed the spread of artemisinin resistance. Elimination became a dirty word after the noisy failures of the 1950s and 60s, and the new strategies look like the same old tactics for controlling malaria, presented under the guise of eradicating it. “They’re prescriptions for inertia,” says White.
Worse, they are channelling funds into ineffective measures. Take insecticide-treated bednets, a mainstay of malaria control. “We’ve had meetings with WHO consultants who said, ‘We don’t want to hear a word against bednets. They always work.’ But how cost-effective are they, and what’s the evidence they work in this region? The mosquitoes here bite early in the evening. And who’s getting malaria? Young men. Are they all tucked up in their bednets by 6 o’clock? No. They’re in the fields and forests. Come on! It’s obvious.”
He says that resources could be better devoted to getting rid of fake drugs and monotherapies where artemisinin is not paired with a partner. That would preserve ACTs for as long as possible. The world also needs better surveillance for resistant parasites. White is helping with that by chairing the World-Wide Anti-Malarial Resistance Network — a global community of scientists who are rapidly collecting data on how quickly patients respond to drugs, the presence of resistance genes, the numbers of fake drugs, and more.
White also wants to know if artemisinin-resistant parasites from South-east Asia can spread in African mosquitoes. Hundreds of mosquito species can transmit malaria, butP. falciparum is picky about its hosts. If resistant strains need time to adapt to new carriers, they might be slow to spread westwards. If they can immediately jump into far-off species, they are a plane ride away from Africa. “That changes your containment strategy,” says White, “but stupidly, it’s cut out of every research application we’ve ever made.”
He is pessimistic. “I’m pretty confident we won’t win but I think we should try a lot harder than we have been. If we didn’t pull out all the stops and kids start dying of artemisinin-resistant malaria, and we can trace the genetic origins of those parasites to South-east Asia, we shouldn’t sleep easy in our beds.”
The Mosquito breederWhen Nosten’s team first arrived at Hka Naw Tah in February, they slept and worked from the village’s unassuming temple. Using development funds from their grant, they put up a water tower and supplied electricity for the local school. In return, the villagers built them a clinic — a spacious, open-sided hut with a sloping tin roof, benches sitting on a dirt floor, a couple of tables holding boxes of drugs and diagnostic kits, treatment rooms, and a computer station. It took just two days to erect.
The Karen respect strong leadership but there is an easy-going camaraderie in the clinic. When we arrive, one of the research assistants is napping across a bench. Nosten walks over and sits on him. “You see, and I think this is a good sign, that it’s hard to tell who’s the boss and who’s the patient,” he says.
Most of the villagers don’t seem sick, but many of them have malaria nonetheless. Until recently, Nosten’s team had always searched for the parasites by examining a drop of blood under a microscope. If someone is sick, you can see and count thePlasmodium in their red blood cells. But in 2010, they started collecting millilitres of blood — a thousand times more than the usual drops — and searching forPlasmodium‘s DNA. Suddenly, the proportion of infected people shot up from 10 — 20 per cent to 60 — 80 per cent. There are three, four, maybe six times as many infected people as he thought.
“We didn’t believe it at first,” says Nosten, “but we confirmed it and re-confirmed it.” Perhaps the tests were giving false positives, or picking up floating DNA from dead parasites? No such luck — when the team treated people with ACTs, the hidden parasites disappeared. They were real.
These ‘sub-microscopic infections’ completely change the game for elimination. Treating the sick is no longer good enough because the disease could bounce back from the hordes of symptomless carriers. The strike will have to be swift and decisive. If it’s half-hearted, the most resistant parasites will survive and start afresh. In malarial zones, you need to treat almost everyone, clearing the parasites they didn’t even know they had. This is Nosten’s goal in the border villages like Hka Naw Tah. He has support from the Bill and Melinda Gates Foundation, one of the few large funders to have truly grasped the urgency of the situation and who are “very much in the mood for elimination”.

Killing the parasites is easy: it just involves three days of ACTs. Getting healthy people to turn up to a clinic and take their medicine is much harder. The team have spent months on engagement and education. The clinic is dotted with posters explaining the symptoms of malaria and the biology of mosquitoes. Earlier this morning, Honey Moon, a Karen woman who is one of Nosten’s oldest colleagues, knocked on the doors of all the absentees from the last round to persuade them to come for tests. As a result, 16 newcomers turned up for treatments, bringing the team closer to the full 393. Nosten is pleased. “In this village, I’m quite optimistic that most people will be free of the parasite,” he says.
Another village down the river is proving more difficult. They are more socially conservative and have a poorer understanding of healthcare. There are two factions of Karen there, one of which is refusing to take part to spite their rivals. “It’s a good lesson for us,” says Nosten. “These situations will be elsewhere.” Eliminating malaria is not just about having the right drug, the deadliest insecticide, or the most sensitive diagnostic test. It is about knowing people, from funders to villagers. “The most important component is getting people to agree and participate,” says Nosten. It matters that he has been working in the region for 30 years, that the Shoklo unit is a familiar and trusted name in these parts, that virtually all his team are Karen. These are the reasons that give Nosten hope, despite the lack of political will.
If the strategy looks like it is working after a year, they will start scaling up. Eventually, they hope to cover the entire sinuous border. I ask Nosten if he would ever consider leaving. He pauses. “Even if I wanted to go somewhere else, I’m more or less a prisoner of my own making,” he says. He would need to find a replacement first — a leader who would command respect among both the Karen and malaria researchers, and would be willing to relocate to a place as remote as Mae Sot. It is hard to imagine a second person who would tick all those boxes. Surrounded by airborne parasites, spreading resistance, and border-hopping refugees, François Nosten is stuck. He would not have it any other way.
Main references
- François Nosten and colleagues describe the three populations of artemisinin-resistantPlasmodium falciparum in Cambodia.
- François Nosten and colleagues study the emergence of artemisinin-resistant malaria on the Thai — Myanmar border.
- Nick White’s 2008 paper raising concerns about artemisinin resistance in Cambodia.
Resources
Contributions
The Shoklo Malaria Research Unit receives funding from the Wellcome Trust, which publishes Mosaic. Dominic Kwiatkowski holds a Wellcome Trust Fellowship.
- Author: Ed Yong
- Editor: Mun-Keat Looi
- Fact checker: Cameron Bird
- Photographer: Ian Teh/Panos
- Copyeditor: Tom Freeman
This article first appeared on Mosaic and is republished here under Creative Commons licence. Mosaic is dedicated to exploring the science of life. Each week, it publishes a feature on an aspect of biology or medicine that affects our lives, our health or our society; it tells stories with real depth about the ideas, trends and people that drive contemporary life sciences. Mosaic is published by the Wellcome Trust, a global charitable foundation that seeks to drive extraordinary improvements in human and animal health. It covers subjects that fit with the Trust’s mission and vision, but isn’t limited to the research the Trust funds.
Images by World Bank Photo Collection, Gates Foundation and US Army Africa
